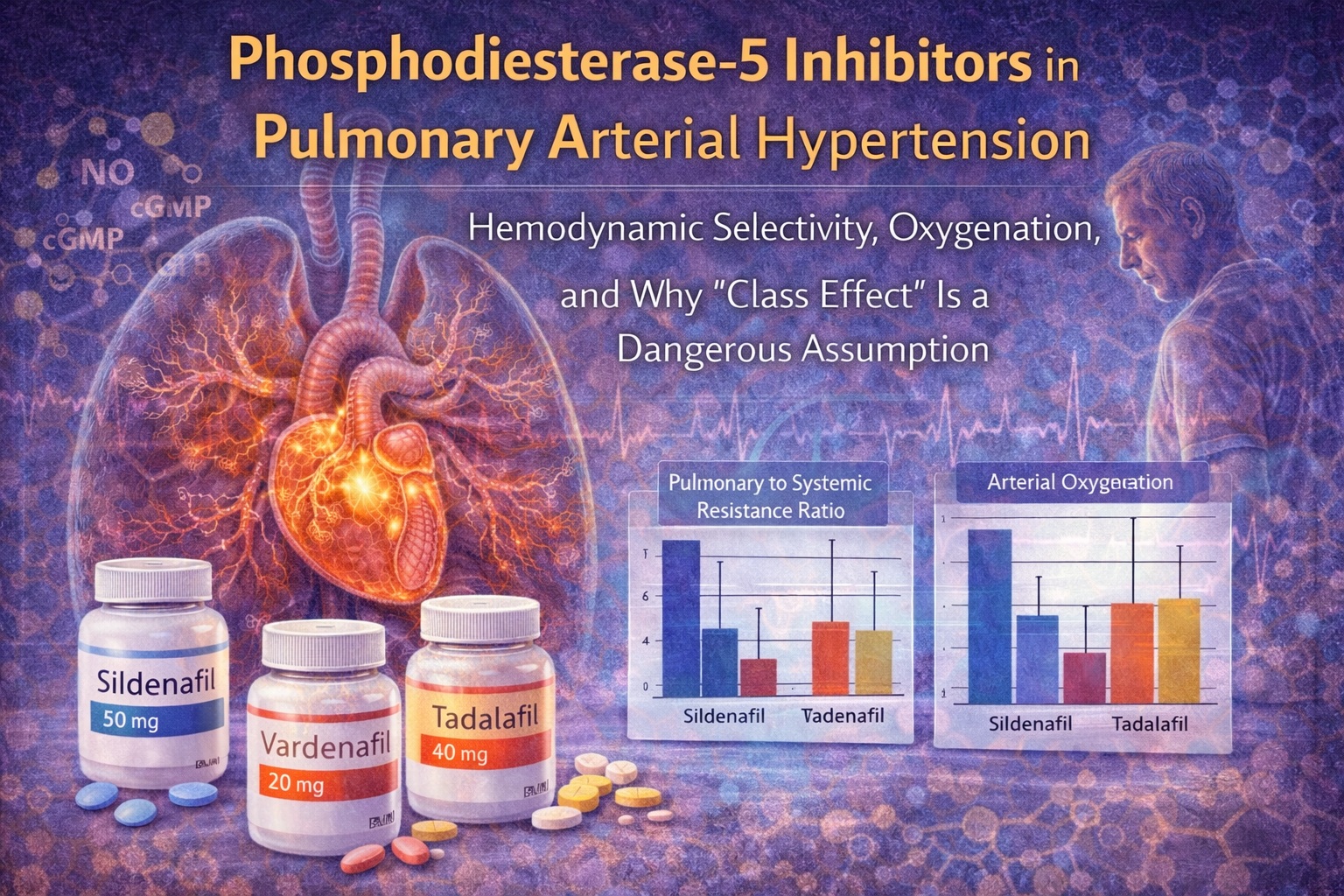
Introduction: When Similar Molecules Behave Very Differently
Pulmonary arterial hypertension (PAH) is a disease defined by precision. Small changes in pulmonary vascular resistance, right ventricular afterload, or oxygenation can translate into large differences in symptoms, functional capacity, and survival. As a result, pharmacological interventions in PAH are judged not only by whether they dilate vessels, but by where, how selectively, and at what physiological cost they do so.
Phosphodiesterase-5 (PDE5) inhibitors entered the PAH field with considerable enthusiasm. Sildenafil demonstrated that oral augmentation of the nitric oxide–cyclic guanosine monophosphate (NO–cGMP) pathway could reproduce many of the benefits of inhaled nitric oxide, but in a practical, long-term form. With the subsequent introduction of vardenafil and tadalafil—agents sharing the same molecular target—it was tempting to assume therapeutic interchangeability.
The study analyzed here decisively challenges that assumption. By directly comparing sildenafil, vardenafil, and tadalafil under controlled hemodynamic conditions, it demonstrates that PDE5 inhibition is not a uniform intervention. Differences in pulmonary selectivity, systemic effects, kinetics, and oxygenation responses are not subtle curiosities—they are clinically meaningful distinctions.
Pulmonary Arterial Hypertension and the Central Role of the NO–cGMP Pathway
The pathophysiology of PAH is characterized by vasoconstriction, vascular remodeling, thrombosis in situ, and progressive right ventricular failure. Among these mechanisms, impaired nitric oxide signaling occupies a central position. Endothelial dysfunction leads to reduced NO bioavailability, diminished activation of soluble guanylate cyclase, and lower intracellular cGMP levels within pulmonary vascular smooth muscle.
PDE5 plays a critical regulatory role by degrading cGMP. In PAH, PDE5 expression and activity are upregulated in pulmonary vascular tissue, further amplifying vasoconstriction and smooth muscle proliferation. Inhibiting PDE5 therefore restores and prolongs cGMP signaling, promoting vasodilation and potentially exerting antiproliferative effects.
Importantly, PDE5 is not exclusive to the pulmonary circulation. It is also expressed in systemic vasculature, myocardium, platelets, and other tissues. This raises a fundamental therapeutic challenge: how to achieve pulmonary vasodilation without provoking systemic hypotension or impairing gas exchange.
Study Design: A Direct Head-to-Head Hemodynamic Comparison
The study enrolled sixty patients with well-characterized chronic PAH across New York Heart Association (NYHA) functional classes II to IV. All patients underwent right heart catheterization, providing a gold-standard assessment of pulmonary and systemic hemodynamics as well as gas exchange parameters.
After baseline measurements, each patient first received inhaled nitric oxide, serving as a physiological reference for pulmonary-selective vasodilation. Once hemodynamics returned to baseline, patients were administered a single oral dose of one PDE5 inhibitor: sildenafil 50 mg, vardenafil 10 or 20 mg, or tadalafil 20, 40, or 60 mg. Hemodynamic and oxygenation variables were then monitored for up to 120 minutes.
This design allowed not only comparison between drugs, but also comparison with an established pulmonary-selective vasodilator. It is precisely this methodological rigor that gives the findings enduring relevance.
Sildenafil: Pulmonary Selectivity with Improved Oxygenation
Sildenafil produced a robust reduction in mean pulmonary arterial pressure and pulmonary vascular resistance, accompanied by a significant increase in cardiac index. Critically, these changes occurred with a relative sparing of systemic vascular resistance, resulting in a favorable reduction of the pulmonary-to-systemic vascular resistance ratio.
Equally important was sildenafil’s effect on gas exchange. Arterial oxygen tension increased significantly, closely mirroring the response observed with inhaled nitric oxide. This suggests not only pulmonary vasodilation, but intrapulmonary selectivity—a preferential redistribution of blood flow toward well-ventilated lung regions.
From a physiological standpoint, this is highly desirable. In PAH, indiscriminate vasodilation can worsen ventilation–perfusion mismatch by increasing perfusion to poorly ventilated areas. Sildenafil appears to avoid this pitfall, amplifying endogenous cGMP signaling in regions where it is already active rather than overriding local regulatory mechanisms.
Vardenafil: Rapid Onset at the Cost of Selectivity
Vardenafil demonstrated the most rapid onset of pulmonary vasodilation among the three agents, with peak effects occurring within approximately 40–45 minutes. From a purely kinetic perspective, this might seem advantageous, particularly in acute settings.
However, this rapid effect came with a critical limitation: lack of pulmonary selectivity. Vardenafil reduced pulmonary and systemic vascular resistance to a similar degree, resulting in little or no improvement in the pulmonary-to-systemic resistance ratio. In practical terms, this means that pulmonary vasodilation was accompanied by parallel systemic vasodilation.
Consistent with this nonselective profile, vardenafil did not improve arterial oxygenation. The absence of oxygenation benefit suggests that vasodilation occurred indiscriminately across the pulmonary circulation, without preferential enhancement of ventilation–perfusion matching.
While systemic side effects were mild in this short-term study, the hemodynamic profile raises concerns regarding the suitability of vardenafil for chronic PAH therapy, where systemic hypotension and impaired gas exchange can have serious consequences.
Tadalafil: Durable Pulmonary Vasodilation Without Oxygenation Gain
Tadalafil displayed a distinctly different profile. Its onset of action was slower, with peak pulmonary vasodilation occurring between 75 and 90 minutes, consistent with its longer half-life and pharmacokinetics. Once established, however, its effects were sustained.
Importantly, tadalafil demonstrated pulmonary selectivity even at higher doses. The pulmonary-to-systemic resistance ratio decreased significantly, indicating preferential action on the pulmonary circulation. This distinguishes tadalafil clearly from vardenafil and aligns it more closely with sildenafil in terms of vascular targeting.
Yet tadalafil differed from sildenafil in a crucial respect: it did not improve arterial oxygenation. Despite effective pulmonary vasodilation, gas exchange parameters remained essentially unchanged. This suggests that tadalafil’s vasodilatory action, while pulmonary-selective at the vascular level, does not enhance ventilation–perfusion matching in the same way as sildenafil.
Kinetics Matter: Timing as a Therapeutic Variable
One of the most instructive aspects of the study is the demonstration that timing itself is a pharmacodynamic variable. Vardenafil acts quickly, sildenafil at an intermediate pace, and tadalafil more slowly but for a longer duration.
In PAH management, these kinetic differences are not academic. Rapid onset may be desirable in acute testing, but sustained effects are essential for chronic therapy. Conversely, delayed peak effects may complicate dose titration or acute response assessment.
The study underscores that pharmacokinetics cannot be separated from pharmacodynamics. A drug’s half-life, tissue distribution, and enzyme selectivity together shape its clinical profile.
Oxygenation as a Discriminator of Clinical Value
Among all measured outcomes, changes in arterial oxygenation may be the most clinically telling. Improvement in oxygenation suggests not only vasodilation, but intelligent vasodilation—one that respects the lung’s intrinsic regulatory architecture.
Sildenafil’s ability to improve oxygenation sets it apart. It implies that sildenafil enhances NO–cGMP signaling preferentially in lung regions with preserved endothelial function and active NO production. In contrast, vardenafil and tadalafil may exert more uniform vasodilation, lacking this intrapulmonary selectivity.
For patients with advanced PAH, where hypoxemia already limits exercise capacity and quality of life, preservation or improvement of oxygenation is not optional—it is essential.
Mechanistic Insights: Why PDE5 Inhibitors Are Not Interchangeable
Despite targeting the same enzyme, sildenafil, vardenafil, and tadalafil differ in their selectivity for other phosphodiesterase isoforms, their tissue penetration, and their interaction with baseline NO signaling. Sildenafil exhibits a unique balance of PDE5 inhibition and amplification of endogenous vasoregulatory loops within the lung.
Differences in affinity for PDE6, PDE1, and PDE11, as well as variations in protein binding and distribution, likely contribute to the divergent profiles observed. These distinctions are often minimized in discussions of erectile dysfunction, but in PAH they become decisive.
The study’s central message is therefore mechanistic as much as clinical: shared molecular targets do not guarantee shared physiological outcomes.
Clinical Implications for PAH Therapy
From a clinical perspective, the findings argue strongly against assuming a “class effect” for PDE5 inhibitors in PAH. Sildenafil emerges as the agent with the most favorable balance of pulmonary selectivity and oxygenation benefit. Tadalafil offers sustained pulmonary vasodilation with acceptable selectivity, making it a plausible alternative, particularly where long duration is desired.
Vardenafil, despite rapid onset, lacks the pulmonary specificity required for safe and effective PAH therapy and should be approached with caution in this context.
These distinctions have implications not only for drug choice, but for guideline development, regulatory evaluation, and future clinical trial design.
Limitations and the Need for Long-Term Data
It is important to recognize that the study evaluates short-term hemodynamic responses. Long-term outcomes such as exercise capacity, right ventricular remodeling, hospitalization, and survival cannot be inferred directly.
Nevertheless, short-term hemodynamics and oxygenation responses are powerful predictors of clinical trajectory in PAH. Drugs that worsen ventilation–perfusion matching or induce systemic hypotension acutely are unlikely to perform well chronically.
Thus, while confirmatory long-term studies are essential, the mechanistic insights provided here remain highly relevant.
Conclusion
This comparative study demonstrates that sildenafil, vardenafil, and tadalafil—despite all being classified as PDE5 inhibitors—exert fundamentally different effects on pulmonary hemodynamics and oxygenation in PAH. Sildenafil uniquely combines pulmonary selectivity with improved arterial oxygenation. Tadalafil offers durable pulmonary vasodilation without oxygenation benefit. Vardenafil, while rapid in onset, lacks pulmonary specificity.
The findings challenge simplistic notions of drug class equivalence and underscore the necessity of individualized pharmacological evaluation in PAH. In a disease where precision matters, assumptions are a luxury clinicians cannot afford.
FAQ
1. Are all PDE5 inhibitors interchangeable in pulmonary arterial hypertension?
No. Despite sharing a molecular target, sildenafil, vardenafil, and tadalafil differ significantly in pulmonary selectivity and oxygenation effects.
2. Why is oxygenation response important in PAH therapy?
Because nonselective vasodilation can worsen ventilation–perfusion mismatch and hypoxemia, offsetting hemodynamic benefits.
3. Does a rapid onset of vasodilation indicate better efficacy?
Not necessarily. Rapid onset without pulmonary selectivity may increase systemic side effects without improving clinical outcomes.