Introduction: The Subtle Art of Treating Symptoms That Define Daily Life
Benign prostatic hyperplasia (BPH) rarely threatens life—but it profoundly shapes how it is lived. For millions of aging men, lower urinary tract symptoms (LUTS) become a daily negotiation: urgency, nocturia, weak stream, incomplete emptying. These are not dramatic complaints, yet they steadily erode quality of life.
Traditionally, treatment has been straightforward. Alpha-blockers such as tamsulosin are prescribed to improve urinary flow, and in many cases, they perform reliably. However, medicine rarely operates in isolation. LUTS and erectile dysfunction (ED) frequently coexist, sharing overlapping pathophysiological pathways and affecting the same patient population.
This is where tadalafil enters the conversation—not as a replacement, but as an alternative with a different philosophy.
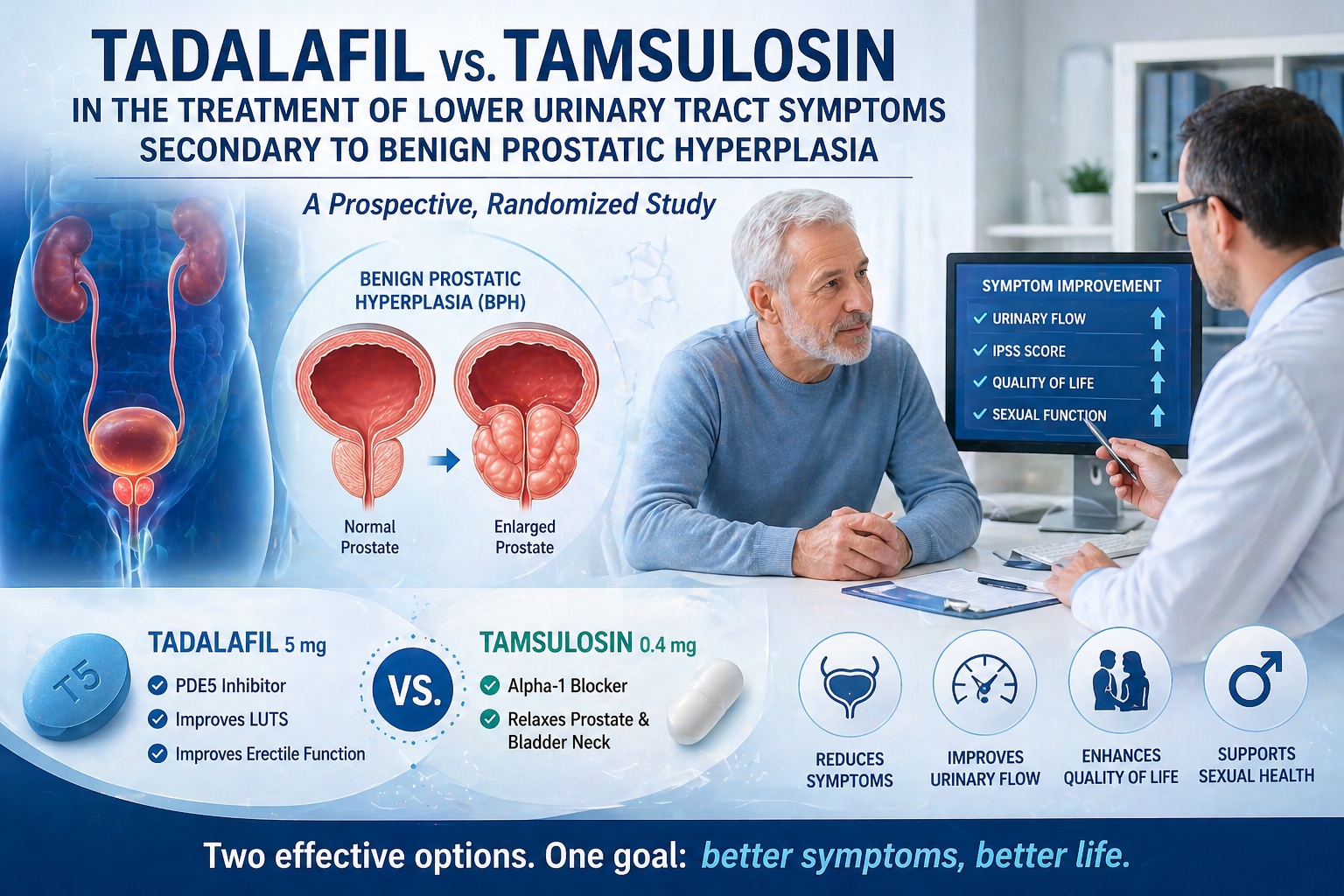
The study provides a direct comparison between tadalafil 5 mg and tamsulosin 0.4 mg in patients with LUTS secondary to BPH. The results are nuanced, clinically relevant, and—perhaps unexpectedly—philosophically revealing.
Understanding LUTS in BPH: More Than a Mechanical Obstruction
At first glance, BPH appears to be a simple mechanical problem: an enlarged prostate compresses the urethra, impairing urine flow. While this explanation is convenient, it is incomplete.
LUTS arise from both static and dynamic components. The static component refers to the physical enlargement of the prostate. The dynamic component, however, involves smooth muscle tone in the prostate and bladder neck, mediated by adrenergic receptors.
Beyond these, there are additional contributors—detrusor overactivity, altered bladder compliance, and even changes in pelvic blood flow. In short, LUTS is not a single disease but a syndrome with multiple drivers.
This complexity explains why different drugs produce different outcomes. Tamsulosin targets the dynamic component directly, while tadalafil operates through vascular and neuromodulatory pathways.
The choice between them is therefore not merely pharmacological—it is conceptual.
Mechanisms of Action: Two Drugs, Two Philosophies
Tamsulosin is a selective alpha-1 adrenergic receptor antagonist. By blocking these receptors, it relaxes smooth muscle in the prostate and bladder neck, facilitating urine flow. The effect is rapid and often measurable.
Tadalafil, in contrast, inhibits phosphodiesterase type 5 (PDE5), increasing cGMP levels and promoting smooth muscle relaxation through nitric oxide signaling. Its effects are more diffuse, influencing not only the prostate but also the bladder, vasculature, and even neural pathways.
As noted in the study, PDE5 inhibitors may reduce detrusor overactivity and improve bladder oxygenation . However, their impact on urinary flow is less direct.
This distinction becomes clinically significant. Tamsulosin improves the mechanics of urination; tadalafil modulates the environment in which those mechanics occur.
Both approaches are valid—but they are not equivalent.
Study Design: A Direct and Practical Comparison
The study enrolled 100 patients with LUTS secondary to BPH, randomized into two groups: tadalafil and tamsulosin. Each group contained 50 patients, and treatment was administered over 12 weeks.
Patients were evaluated using multiple clinically relevant parameters:
- Maximum urinary flow rate (Qmax)
- Postvoid residual urine (PVR)
- International Prostate Symptom Score (IPSS)
- Quality of life (IPSS QoL)
- Sexual Health Inventory for Men (SHIM)
Assessments were conducted at baseline, 1 week, 4 weeks, and 12 weeks, providing a dynamic view of treatment response .
Importantly, baseline characteristics were comparable between groups, ensuring that differences in outcomes reflected treatment effects rather than patient variability.
Urinary Outcomes: Where Tamsulosin Takes the Lead
The results are clear in one domain: urinary flow.
After 12 weeks, both drugs improved Qmax, but the improvement was significantly greater with tamsulosin. The mean increase was +4.0 ml/sec in the tamsulosin group compared to +2.4 ml/sec with tadalafil (p = 0.002) .
Similarly, reduction in postvoid residual urine was more pronounced with tamsulosin (−59 ml vs. −12 ml, p = 0.004).
These findings reflect the drug’s mechanism. By directly relaxing the bladder outlet, tamsulosin enhances urine flow efficiently and predictably.
Tadalafil, while beneficial, appears less potent in this regard. Its indirect mechanism may limit its ability to produce dramatic improvements in flow metrics.
For patients whose primary concern is urinary obstruction, the choice is straightforward.
Symptom Scores and Quality of Life: A More Nuanced Picture
When examining symptom scores, the difference becomes less pronounced.
Both drugs improved IPSS, but the reduction was greater with tamsulosin (−2.76 vs. −0.62), though not statistically significant .
Quality of life scores improved in both groups, again without significant differences.
This suggests that while tamsulosin improves objective measures more effectively, subjective symptom relief may be comparable between treatments.
In clinical practice, this distinction matters. Patients do not measure Qmax at home—they measure comfort, convenience, and disruption.
In that sense, tadalafil holds its ground.
Sexual Function: Where Tadalafil Redefines the Equation
The most striking difference between the two drugs lies in sexual health.
In patients with concomitant erectile dysfunction, tadalafil produced a statistically significant improvement in SHIM scores (+2.88, p = 0.001), while tamsulosin did not (+1.24, p = 0.217) .
This is not surprising—tadalafil was designed for this purpose. However, its dual effect on LUTS and ED creates a unique therapeutic advantage.
For patients experiencing both conditions, tadalafil addresses two problems with one intervention. This is not merely convenient—it is transformative.
It shifts treatment from symptom management to holistic care.
Interpreting the Trade-Off: Flow vs. Function
The comparison between tadalafil and tamsulosin ultimately reflects a trade-off.
Tamsulosin excels in improving urinary flow and reducing residual urine. It is efficient, targeted, and reliable.
Tadalafil, while less potent in these parameters, offers broader benefits—particularly in sexual function and overall well-being.
This creates a clinical decision point:
- If urinary obstruction is the dominant issue, tamsulosin is likely the better choice.
- If erectile dysfunction is present or quality of life is the priority, tadalafil becomes highly attractive.
In some cases, combination therapy may provide the best of both worlds—a strategy supported by emerging evidence.
Safety and Tolerability: A Quiet Strength
Both drugs were well tolerated in the study, with minimal adverse events .
This is an important consideration. In chronic conditions such as BPH, long-term adherence is essential. Drugs that are effective but poorly tolerated rarely succeed in practice.
The comparable safety profiles of tadalafil and tamsulosin allow clinicians to focus on efficacy and patient preference rather than risk.
In this sense, the choice becomes not about safety—but about strategy.
Clinical Implications: Personalizing Treatment
The study reinforces a fundamental principle of modern medicine: treatment should be individualized.
BPH is not a uniform condition, and patients are not interchangeable. Age, comorbidities, symptom profile, and personal priorities all influence the optimal choice of therapy.
Tadalafil introduces flexibility into this equation. It allows clinicians to address overlapping conditions and tailor treatment to the patient’s broader experience.
In practice, this means asking better questions:
What bothers the patient most?
What are their expectations?
What outcomes matter to them?
The answers will often guide the prescription more effectively than any algorithm.
Conclusion: Two Paths, One Goal
Tadalafil and tamsulosin represent two valid approaches to the same problem.
One focuses on restoring flow; the other on restoring function.
The study demonstrates that while tamsulosin may be more effective in improving objective urinary parameters, tadalafil offers meaningful benefits in sexual health and overall quality of life.
Neither drug is universally superior. Each has its place.
The art of treatment lies in choosing the right one—or combining them—based on the patient in front of you.
Because in the end, success is not defined by numbers on a chart, but by the patient’s ability to live comfortably, confidently, and fully.
FAQ: Practical Questions About Tadalafil vs. Tamsulosin
1. Which drug is better for urinary symptoms?
Tamsulosin generally provides greater improvement in urinary flow and residual urine.
2. Does tadalafil help with BPH symptoms?
Yes, but its effect is more modest compared to tamsulosin.
3. Which drug improves erectile dysfunction?
Tadalafil significantly improves erectile function; tamsulosin does not.
4. Can both drugs be used together?
Yes, combination therapy may offer enhanced benefits in selected patients.
5. How should treatment be chosen?
Based on symptom profile, presence of ED, and patient preferences.