Introduction: Erectile Dysfunction as a Vascular Warning Signal
Erectile dysfunction is often discussed as a quality-of-life disorder, but that description is incomplete. For many men, ED is not simply a local problem of penile blood flow; it is an early visible sign of a deeper vascular process. The penile arteries are small, sensitive, and unforgiving. When endothelial health begins to decline, they may complain before the coronary arteries do. In that sense, ED sometimes behaves like a cardiologist’s whisper before the cardiologist has even entered the room.
The study “Tadalafil treatment had a modest effect on endothelial cell damage and repair ability markers in men with erectile dysfunction and vascular risk” explores this important biological connection. The investigators examined whether tadalafil, a selective phosphodiesterase type 5 inhibitor, could do more than improve erection. They asked a more ambitious question: can tadalafil also improve laboratory markers of endothelial damage and vascular repair capacity in men with ED and vascular risk factors?
This question matters because the endothelium is not just a passive lining inside blood vessels. It is a dynamic organ that regulates vascular tone, inflammation, coagulation, platelet activity, and tissue repair. When the endothelium becomes dysfunctional, the consequences extend far beyond erection. They touch atherosclerosis, cardiovascular risk, and long-term vascular resilience.
Tadalafil is clinically effective for many men with ED because it enhances nitric oxide–mediated cyclic guanosine monophosphate signaling, allowing smooth muscle relaxation and improved cavernosal blood flow. However, a drug that improves erectile performance does not automatically repair vascular biology. This study is valuable precisely because it tests that distinction. It separates functional improvement from deeper endothelial recovery, and the result is clinically sobering: tadalafil improved erectile function, but its effect on endothelial repair markers was modest.
Endothelial Dysfunction: The Hidden Architecture Behind Erectile Failure
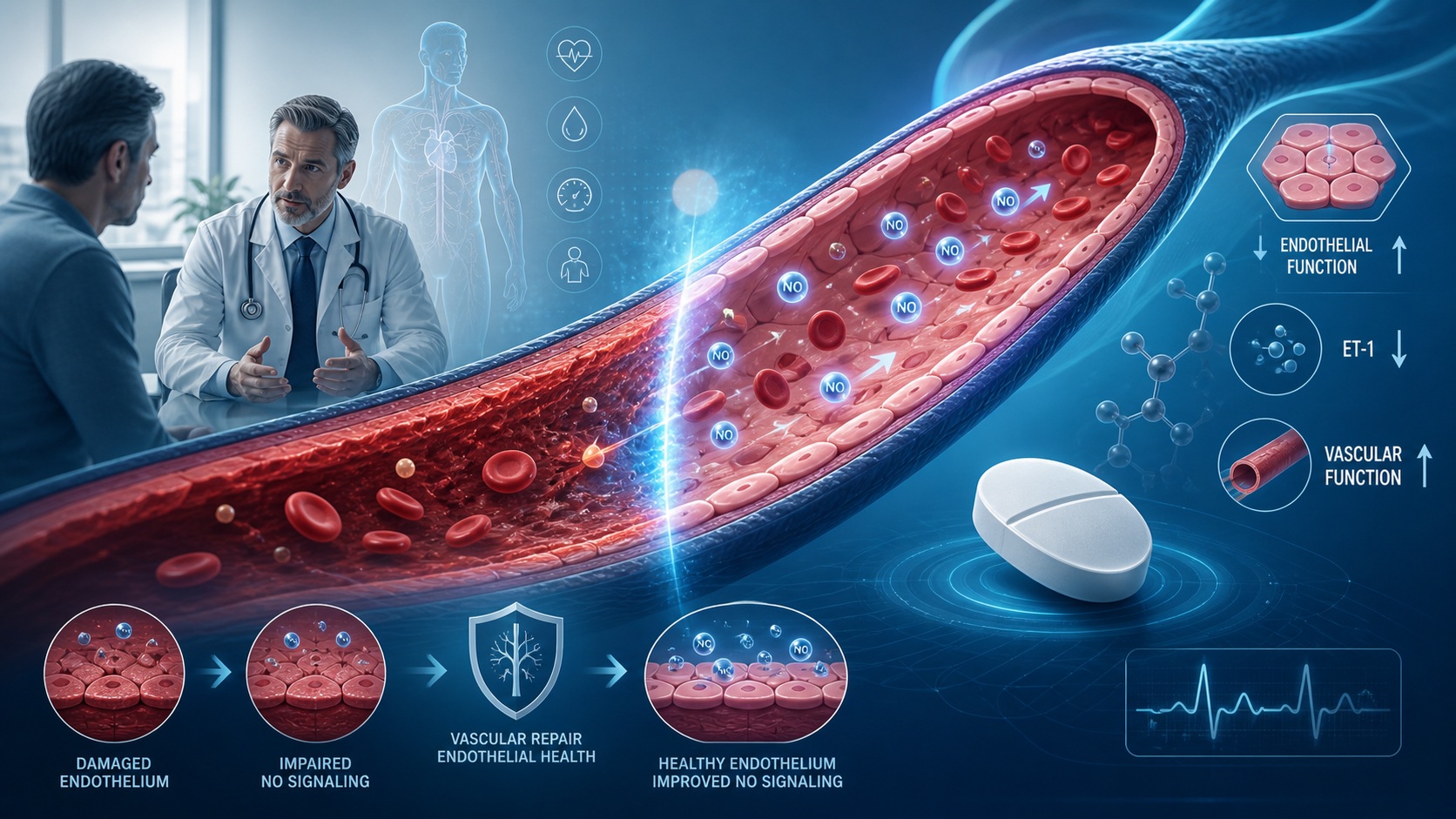
To understand the significance of the study, one must first understand the endothelium. Healthy endothelial cells release nitric oxide, maintain vascular flexibility, inhibit excessive inflammation, and prevent abnormal clot formation. When vascular risk factors such as diabetes, hypertension, obesity, dyslipidemia, and smoking accumulate, endothelial cells become stressed. They lose part of their protective function and begin releasing biochemical signals that reflect vascular damage.
In men with ED and vascular risk factors, this endothelial injury becomes clinically relevant. Erectile function depends on rapid vascular relaxation and adequate arterial inflow into the corpora cavernosa. If endothelial nitric oxide production is impaired, the erectile response becomes weaker, less reliable, and less sustainable. The patient experiences this as ED, while the clinician should also recognize it as a possible vascular warning sign.
The study focused on markers of endothelial cell damage and repair. These included endothelin-1, soluble E-selectin, tissue-type plasminogen activator, circulating angiogenic cells, and colony-forming units. These terms may sound like laboratory poetry written by someone with no interest in readability, but they are important. They help describe whether the vascular system is inflamed, constricted, prothrombotic, or capable of repair.
Endothelin-1 is a powerful vasoconstrictor. When elevated, it suggests a vascular environment leaning toward constriction and dysfunction. Soluble E-selectin reflects endothelial activation and inflammatory signaling. Tissue-type plasminogen activator is related to fibrinolysis and endothelial-associated thrombotic balance. Circulating angiogenic cells and colony-forming units serve as laboratory surrogates for vascular repair ability. In simpler language, they help answer this question: can the vascular system repair itself after damage?
The investigators had previously shown that serum from men with ED and vascular risk factors could inhibit the development of circulating angiogenic cells and colony-forming units from healthy men’s blood mononuclear cells. This suggests that the serum of such patients contains factors that actively suppress endothelial repair. That concept is particularly important. It means ED is not only a symptom of impaired blood flow; it may reflect a systemic biochemical environment hostile to vascular recovery.
What the Study Did: Tadalafil, Placebo, and the Search for Repair
The study enrolled 36 men with ED and vascular risk factors. These participants were randomized to receive either tadalafil 20 mg every other day or placebo for four weeks. A group of healthy men without ED or recognized vascular risk factors served as controls. The design was small but focused, aiming to examine whether tadalafil could alter the serum environment that impairs endothelial repair.
Erectile function was assessed using the Sexual Health Inventory for Men. Laboratory testing evaluated endothelial damage markers and the ability of patient serum to influence circulating angiogenic cells and colony-forming units derived from healthy men. This is a clever experimental model because it does not merely measure cells circulating in the patient’s body; it asks whether the patient’s serum itself promotes or suppresses vascular repair.
At baseline, men with ED differed significantly from healthy controls. They had higher body mass index, larger waist circumference, higher blood pressure, higher fasting glucose, higher cholesterol, greater carotid intima-media thickness, and lower erectile function scores. These findings are clinically predictable but still important. They confirm that the ED group was not merely sexually symptomatic; it carried a measurable vascular risk burden.
The page 3 figure in the paper visually summarizes the main results: tadalafil improved erectile function scores and reduced endothelin-1 and tissue-type plasminogen activator levels, but did not meaningfully change soluble E-selectin or the inhibitory effect of patient serum on circulating angiogenic cells and colony-forming units. This visual pattern captures the central message of the article: function improved, but vascular repair biology remained largely resistant.
The treatment was generally tolerated, and no participants receiving tadalafil discontinued because of adverse events. This is consistent with the known safety profile of tadalafil in appropriately selected patients. Yet safety and efficacy for erection are not the same as endothelial restoration. Medicine often enjoys simple narratives, but biology rarely signs the contract.
The Main Findings: Better Erections, Modest Endothelial Change
The most clinically obvious finding was that tadalafil improved erectile function. The Sexual Health Inventory for Men score increased significantly after tadalafil therapy compared with baseline and placebo. This confirms what clinicians already know: tadalafil can be effective in men with ED, including those with vascular risk factors.
The more interesting finding lies in what tadalafil did not do. It did not reverse the inhibitory effect of serum from ED patients on circulating angiogenic cells or colony-forming units derived from healthy men. In practical terms, tadalafil did not meaningfully improve the serum-mediated repair environment within the short treatment period. The vascular repair machinery remained impaired.
This distinction is crucial. A man may experience better erectile function because tadalafil amplifies nitric oxide–cGMP signaling, improves smooth muscle relaxation, and enhances blood inflow during sexual stimulation. However, this does not necessarily mean that the underlying vascular risk state has been corrected. The drug improves the performance of the system, but it may not rebuild the system.
Tadalafil did reduce endothelin-1 levels. This is biologically plausible because PDE5 inhibition can influence endothelial signaling and vascular tone. Lower endothelin-1 may indicate a shift away from excessive vasoconstriction. That is favorable, but the clinical significance remains uncertain. A biomarker improvement is not automatically a cardiovascular outcome improvement.
The study also found a reduction in tissue-type plasminogen activator after tadalafil treatment. Since baseline tPA levels were not significantly different between ED patients and controls, this finding requires caution. It may reflect a favorable change in endothelial-associated prothrombotic balance, or it may simply be a signal that needs confirmation in larger studies.
Soluble E-selectin did not significantly change. This matters because E-selectin reflects endothelial activation and inflammatory signaling. If tadalafil had broadly improved endothelial injury, one might expect a decrease in this marker. The absence of change supports the authors’ conclusion that tadalafil’s effect on endothelial damage and repair markers was limited.
Clinical Meaning: What Physicians and Patients Should Actually Learn
The clinical lesson is not that tadalafil is weak. The lesson is that tadalafil is specific. It is effective at improving erectile function through a defined vascular mechanism, but it should not be mistaken for a full vascular rehabilitation program. That distinction protects patients from unrealistic expectations and protects clinicians from therapeutic overstatement.
For men with ED and vascular risk factors, tadalafil may restore sexual confidence and improve quality of life. That benefit is meaningful. Sexual function is not a decorative luxury; it affects self-esteem, relationships, mood, and overall well-being. However, the presence of ED in a man with metabolic or cardiovascular risk factors should trigger broader evaluation, not merely a prescription.
This study reinforces the importance of treating the vascular terrain. Blood pressure control, lipid management, glucose optimization, smoking cessation, weight reduction, physical activity, and diet remain central. Tadalafil may help the erectile response, but it does not erase the vascular consequences of years of endothelial exposure to risk factors. It is a therapy, not a moral pardon from the endothelium.
The findings also help refine the discussion around PDE5 inhibitors and cardiovascular health. Some earlier studies suggested that PDE5 inhibition may improve endothelial function or increase circulating angiogenic cells. This study does not deny that possibility, but it adds caution. Benefits may depend on treatment duration, patient selection, dosing schedule, baseline risk burden, and the specific markers used.
In clinical practice, this means that tadalafil should be positioned accurately. It is a first-line pharmacological option for ED in many men and may have some favorable vascular biomarker effects, particularly involving endothelin-1. But it should not be marketed mentally—or medically—as a comprehensive endothelial repair drug. The temptation to turn every positive biomarker into a grand therapeutic narrative is understandable. It is also how medicine occasionally gets ahead of itself.
Why the Results Were Modest: Biology, Risk Factors, and Time
There are several reasons why tadalafil’s endothelial effects may have appeared modest. First, the study duration was short. Four weeks may be enough to improve erectile function, but it may not be enough to reverse years of vascular injury. Endothelial dysfunction develops over time, and vascular repair capacity is shaped by chronic metabolic and inflammatory exposure.
Second, the patients had multiple vascular risk factors. The study population had higher waist circumference, blood pressure, fasting glucose, cholesterol, and carotid intima-media thickness than controls. These are not minor background details. They represent the biological load that continuously injures the endothelium. A PDE5 inhibitor may improve nitric oxide signaling, but it does not remove hyperglycemia, hypertension, dyslipidemia, or visceral adiposity.
Third, the serum inhibition of angiogenic cell development may be driven by unidentified soluble factors not directly affected by tadalafil. The authors suggest that vascular risk factor exposure may create a serum environment that suppresses vascular repair. If so, improving erectile hemodynamics alone would not necessarily normalize repair biology.
Fourth, endothelial repair is complex. Circulating angiogenic cells and colony-forming units are useful laboratory surrogates, but they do not capture the entire repair process. Vascular health involves bone marrow mobilization, inflammatory signaling, oxidative stress, nitric oxide availability, endothelial progenitor function, platelet behavior, and local tissue microenvironment. Expecting one drug to normalize all of this in four weeks would be optimistic. Charming, perhaps, but optimistic.
Finally, the study was small. With only 36 ED patients, it was designed more as an exploratory mechanistic study than a definitive clinical trial. Small studies can reveal signals, but they cannot settle large clinical questions. The modest findings should therefore be interpreted carefully: not dismissed, but not exaggerated.
Toward a More Complete Approach to Erectile and Vascular Health
A modern approach to ED should begin by asking why the dysfunction exists. In younger men, psychogenic factors may dominate. In older men or men with vascular risk factors, ED often reflects endothelial dysfunction and impaired vascular responsiveness. The prescription pad is useful, but it is not a diagnostic strategy.
Tadalafil can play a central role in treatment. Its long half-life, clinical efficacy, and patient acceptance make it a valuable option. In some men, regular dosing may provide greater confidence and a more natural sexual rhythm. In others, on-demand dosing may be sufficient. The key is individualization.
However, men with vascular risk factors need more than erection support. They need cardiovascular risk assessment. ED may precede clinically apparent coronary artery disease, and ignoring that signal is a missed opportunity. The penis, inconveniently for the shy patient, may sometimes be the first organ to report vascular trouble.
Lifestyle intervention should not be presented as a vague moral lecture. It should be explained biologically. Weight reduction improves inflammatory tone and endothelial function. Exercise increases nitric oxide bioavailability and vascular responsiveness. Smoking cessation reduces oxidative endothelial injury. Better glycemic control reduces microvascular damage. These interventions are not “natural alternatives” to tadalafil; they address the disease environment in which tadalafil must work.
Future studies should examine whether longer tadalafil treatment, different dosing strategies, or combination approaches with aggressive vascular risk modification can produce stronger improvements in endothelial repair markers. The most meaningful research will use clinical vascular outcomes, not only surrogate markers. Biomarkers are useful headlights, but they are not the destination.
Conclusion: A Useful Drug, a Clear Limit, and a Better Clinical Message
The study provides a nuanced and clinically responsible message. Tadalafil improved erectile function in men with ED and vascular risk factors, and it reduced certain endothelial-related markers such as endothelin-1 and tissue-type plasminogen activator. However, it did not correct the impaired serum-mediated endothelial repair capacity measured through circulating angiogenic cells and colony-forming units.
This is not disappointing; it is clarifying. Tadalafil does what it is designed to do well: it improves erectile physiology. It may also exert modest favorable effects on selected vascular biomarkers. But it should not be viewed as a stand-alone solution for endothelial dysfunction or vascular risk.
The deeper lesson is that ED must be treated as both a sexual medicine issue and a vascular medicine opportunity. A man who presents with ED and vascular risk factors deserves effective symptom treatment, but he also deserves a serious evaluation of cardiometabolic health.
In the best version of clinical care, tadalafil restores confidence while the physician addresses the vascular roots. One helps the moment. The other protects the future.
FAQ
Does tadalafil improve endothelial function in men with erectile dysfunction?
Tadalafil may improve selected markers of endothelial activity, such as endothelin-1, but this study found only a modest effect overall. It improved erectile function clearly, yet did not restore laboratory measures of endothelial repair capacity.
What are circulating angiogenic cells and why do they matter?
Circulating angiogenic cells are cells involved in vascular repair. A lower ability to generate these cells suggests impaired endothelial repair potential, which may be relevant in men with ED and vascular risk factors.
Does better erectile function mean better cardiovascular health?
Not necessarily. Improved erections after tadalafil show improved erectile response, but they do not automatically prove that systemic vascular health has been restored.
Should men with ED and vascular risk factors take tadalafil?
Tadalafil can be an effective treatment option when prescribed appropriately. However, men with ED and vascular risk factors should also receive cardiovascular and metabolic evaluation.
Can lifestyle changes improve the effect of tadalafil?
Yes, they may. Exercise, weight control, smoking cessation, blood pressure management, lipid control, and diabetes treatment can improve endothelial health and may support better long-term erectile outcomes.