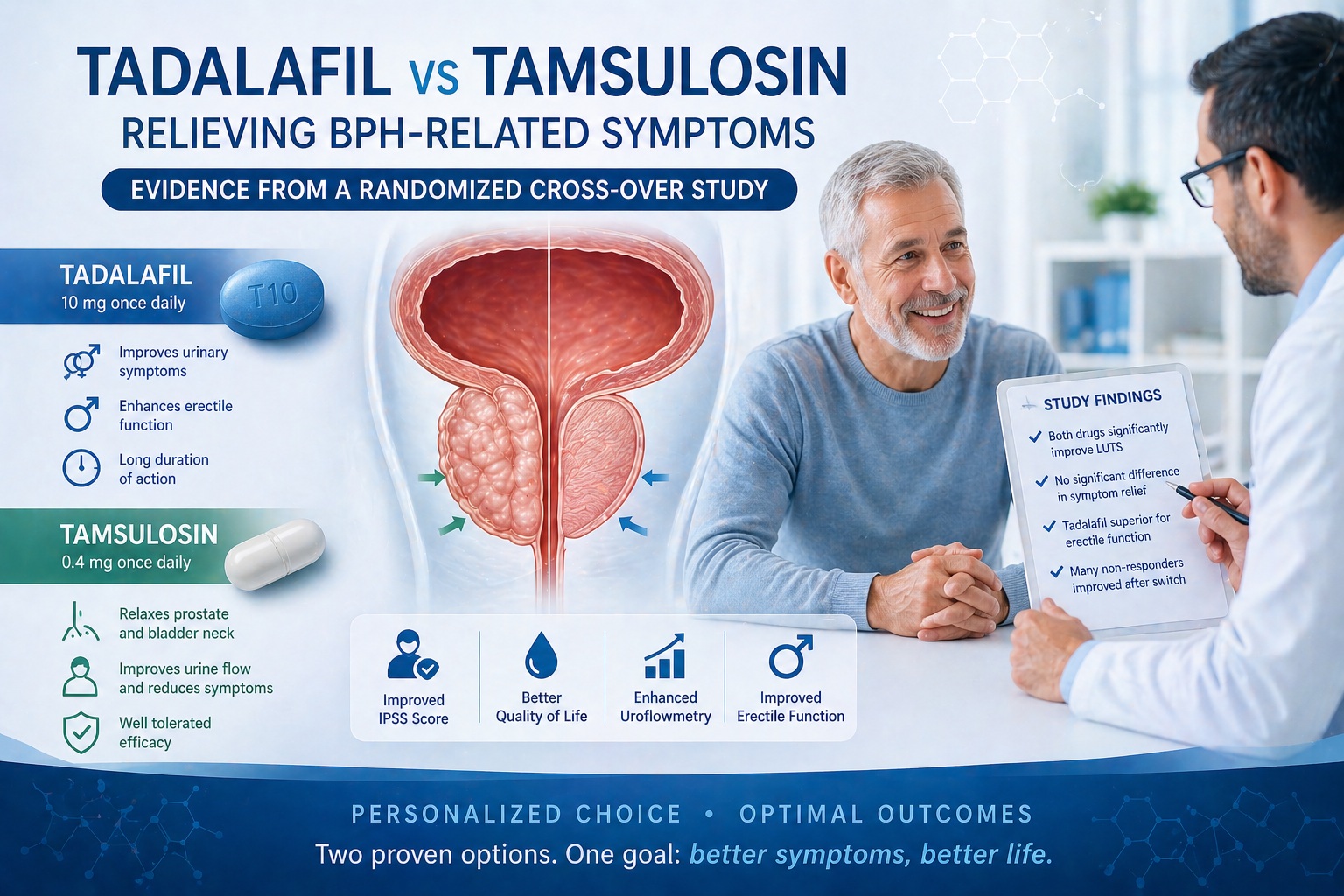
Introduction: When Urinary Symptoms Tell a Bigger Story
Benign prostatic hyperplasia (BPH) is often introduced in textbooks as a simple enlargement of the prostate gland leading to urinary obstruction. In reality, it is far more nuanced. Lower urinary tract symptoms (LUTS) associated with BPH represent a complex interplay between bladder function, smooth muscle tone, neural signaling, and vascular health.
What makes the clinical picture even more intricate is the frequent coexistence of erectile dysfunction (ED). These two conditions—once treated in isolation—are now recognized as overlapping syndromes with shared pathophysiological pathways. The aging male patient rarely presents with one without the other.
The study explores a clinically relevant question: How do two fundamentally different drug classes—tadalafil and tamsulosin—compare when used in the same patients?
This article builds on that investigation, offering a comprehensive, practical, and clinically oriented interpretation of the findings, while expanding the discussion into real-world therapeutic strategy.
Pathophysiological Intersection: Why LUTS and ED Often Walk Together
The coexistence of LUTS and ED is not coincidental. Epidemiological studies consistently show a strong correlation between symptom severity and sexual dysfunction, independent of age and comorbidities .
Four key mechanisms are believed to link these conditions:
- Impaired nitric oxide signaling
- Increased smooth muscle tone in the prostate and bladder neck
- Autonomic nervous system dysregulation
- Pelvic atherosclerosis and reduced blood flow
These overlapping pathways explain why medications targeting one system often influence the other.
From a clinical perspective, this is both a challenge and an opportunity. Treating LUTS without addressing ED may leave the patient dissatisfied. Conversely, improving erectile function without relieving urinary symptoms is equally incomplete.
This duality sets the stage for comparing tadalafil—a PDE5 inhibitor—with tamsulosin—an alpha-1 adrenergic blocker.
Study Design Insights: Why the Cross-Over Model Matters
The study employed a randomized, double-blind, placebo-controlled cross-over design—a methodology that deserves attention in its own right.
Patients aged 45 years and older with moderate to severe LUTS (IPSS ≥8) were assigned to receive either tadalafil or tamsulosin first, followed by a washout period and subsequent crossover to the alternative therapy .
This design offers several advantages:
- Each patient acts as their own control
- Inter-individual variability is minimized
- Direct comparison between therapies becomes more precise
However, it also revealed an important nuance: a significant “period effect.” Symptoms did not fully return to baseline after washout, suggesting either prolonged drug action or psychological carryover effects.
In practical terms, this reminds clinicians that therapeutic effects—especially subjective ones—rarely reset neatly between interventions.
Efficacy in LUTS: A Tie That Demands Interpretation
Both tadalafil and tamsulosin demonstrated statistically significant improvements in LUTS, as measured by the International Prostate Symptom Score (IPSS) .
Interestingly, the magnitude of improvement between the two drugs was not significantly different.
This finding challenges traditional assumptions. Alpha-blockers like tamsulosin have long been considered the gold standard for LUTS. Yet tadalafil, originally developed for ED, performs comparably in this domain.
Several observations from the study deserve emphasis:
- Approximately 70% of patients achieved clinically meaningful improvement
- Both drugs reduced total IPSS and improved quality of life
- Objective measures (e.g., flow rate) showed limited change
The last point is particularly important. Symptom relief does not always correlate with measurable urodynamic improvement. In other words, patients feel better—even if the numbers don’t change dramatically.
This highlights a fundamental principle of clinical medicine: patient perception is often the most meaningful endpoint.
Erectile Function: Where Tadalafil Clearly Leads
While both drugs improved LUTS, their effects on erectile function diverged.
Tadalafil demonstrated superior improvement in IIEF (International Index of Erectile Function) scores compared to tamsulosin .
This is not surprising, given its mechanism of action. By enhancing nitric oxide–mediated vasodilation, tadalafil directly targets the vascular component of erection.
However, the study revealed an intriguing nuance: even tamsulosin produced modest improvements in erectile function.
This raises an important hypothesis—improving urinary symptoms may indirectly enhance sexual performance by:
- Reducing discomfort and anxiety
- Improving sleep quality
- Enhancing overall well-being
Still, when erectile function is a primary concern, tadalafil remains the more reliable choice.
Responder Variability: The Case for Therapeutic Flexibility
One of the most clinically valuable findings of the study is often overlooked: nonresponders to one drug frequently responded to the other.
Approximately half of the patients who did not respond to tadalafil showed improvement after switching to tamsulosin—and vice versa .
This observation carries significant practical implications.
It suggests that:
- Lack of response does not indicate treatment failure
- Switching drug class is a rational next step
- Individual variability outweighs theoretical superiority
In an era increasingly focused on personalized medicine, this finding reinforces a simple but powerful idea: the best drug is the one that works for the patient in front of you.
Safety and Tolerability: Predictable, Manageable, Acceptable
Both medications were generally well tolerated.
Tadalafil was associated with:
- Epigastric discomfort
- Myalgia
- Occasional calf pain
- Mild systemic symptoms
Tamsulosin, on the other hand, showed fewer adverse effects but included:
- Orthostatic hypotension (in rare cases)
- Fatigue
Importantly, most adverse events were mild and self-limiting .
From a clinical standpoint, safety profiles should guide—not dictate—drug selection. Patient comorbidities, tolerance, and preferences must always be considered.
Clinical Strategy: Choosing Between Tadalafil and Tamsulosin
The study does not declare a winner—and that is precisely its strength.
Instead, it provides a framework for decision-making.
Tadalafil may be preferred when:
- ED is present or suspected
- The patient values sexual function highly
- A dual therapeutic effect is desired
Tamsulosin may be preferred when:
- Urinary symptoms are severe and predominant
- Rapid symptom relief is needed
- PDE5 inhibitors are contraindicated
In many cases, combination therapy may offer additive benefits, though this was not the primary focus of the study.
The key is not rigid adherence to guidelines, but thoughtful application of evidence.
Limitations and Interpretation: Reading Between the Lines
No study is without limitations, and this one is no exception.
Key constraints include:
- Small sample size
- Short duration of treatment periods
- Incomplete washout between therapies
- Lack of prostate volume assessment
These factors limit generalizability but do not diminish clinical relevance.
If anything, they highlight the need for larger, more comprehensive trials—particularly in diverse populations.
Conclusion: From Comparison to Personalization
The comparison between tadalafil and tamsulosin is not a competition—it is a conversation.
Both drugs are effective. Both improve quality of life. Both have a place in modern urology.
What differentiates them is not efficacy alone, but context.
Tadalafil stands out for its dual action—addressing both LUTS and erectile dysfunction. Tamsulosin remains a reliable, targeted therapy for urinary symptoms.
The study ultimately reinforces a central truth of medicine:
Treatment success lies not in choosing the “best” drug, but in choosing the right drug for the right patient.
FAQ: Practical Questions Clinicians and Patients Ask
1. Is tadalafil as effective as tamsulosin for urinary symptoms?
Yes, both drugs show comparable improvement in LUTS, although their mechanisms differ.
2. Which drug is better if erectile dysfunction is present?
Tadalafil is superior in improving erectile function while also relieving urinary symptoms.
3. What should be done if one drug does not work?
Switching to the alternative drug is a valid and often effective strategy.
4. Are these drugs safe for long-term use?
Both have favorable safety profiles, but long-term use should be guided by clinical evaluation.
5. Can tadalafil and tamsulosin be used together?
Yes, combination therapy may provide additive benefits in selected patients under medical supervision.