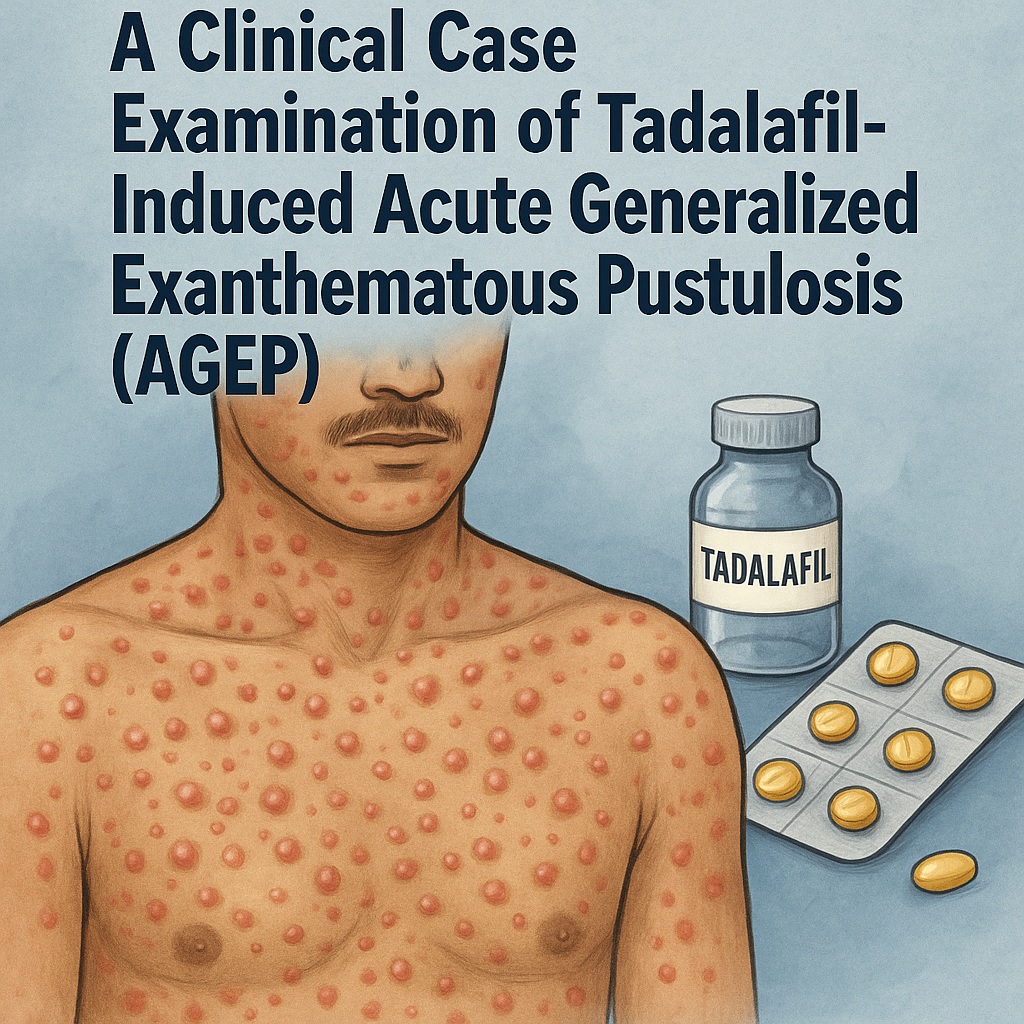
Acute generalized exanthematous pustulosis (AGEP) is a fascinating and intimidating dermatologic emergency—one that many clinicians may hear about but few will actually encounter in practice. This rare form of severe cutaneous adverse reaction (SCAR) typically arises abruptly, progresses rapidly, and often sends clinicians racing down a diagnostic corridor crowded with life-threatening differentials such as pustular psoriasis, Stevens–Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), and drug reaction with eosinophilia and systemic symptoms (DRESS).
The case presented in the uploaded clinical report is particularly noteworthy because AGEP was triggered by a medication not commonly implicated in SCARs: tadalafil. While phosphodiesterase type-5 inhibitors have long been considered safe, well-tolerated, and devoid of significant dermatologic toxicity, this case demonstrates that even the most benign-appearing pharmacologic agents can occasionally provoke dramatic immunologic overreactions.
The goal of this article is to carefully dissect the clinical case, contextualize it within the broader knowledge of AGEP pathophysiology, examine diagnostic challenges, and outline rational management strategies. This analysis adheres strictly to the clinical evidence provided, yet interprets it through a broader academic lens—providing the depth and precision expected of high-level medical commentary.
Clinical Presentation: A Sudden Eruption with a Characteristic—but Easily Misinterpreted—Pattern
The patient described in the report developed a sudden onset of innumerable pustules on an erythematous base, distributed diffusely across the body shortly after ingestion of tadalafil. The temporal relationship was both clinically compelling and diagnostically dangerous: rapid onset of pustules can mimic a surprising number of dermatologic entities, many of which demand vastly different treatments.
AGEP typically presents within hours to days after exposure to a triggering agent. The morphology—a background of widespread erythema studded with pinhead-sized, non-follicular sterile pustules—is distinctive once recognized, but misleading if not. Fever is common; leukocytosis is expected; signs of systemic inflammation are often present; edema of the face may appear; but mucosal involvement, if present at all, is mild.
In this case, the patient’s constellation of symptoms aligned with classic AGEP: rapid progression, pustular eruption, systemic inflammatory markers, and regression after withdrawal of the offending drug. No mucosal erosions or bullae were reported, supporting the diagnosis and helping exclude Stevens–Johnson syndrome.
Clinicians must appreciate how the pace of evolution distinguishes AGEP from pustular psoriasis (gradual) and from SJS/TEN (slower onset, with mucosal injury and necrosis). Recognizing this temporal pattern can prevent dangerous diagnostic missteps.
Diagnostic Reasoning: Applying EUROSCAR and Naranjo Criteria
Diagnosing AGEP is both an art and a science. The EUROSCAR scoring system provides a structured method to determine how strongly a clinical eruption aligns with AGEP. It considers:
- type and distribution of pustules,
- presence of fever,
- neutrophilia,
- timing of onset relative to drug exposure,
- resolution after withdrawal of the agent,
- histopathologic features.
In this case, every major criterion aligned with a definite AGEP diagnosis. The timing after tadalafil exposure was appropriate, the morphology was classic, and recovery occurred after cessation of the drug—forming a robust causal narrative.
Complementing EUROSCAR, the Naranjo adverse drug reaction probability scale offers a pharmacologic causality assessment. In this case, Naranjo scoring yielded a classification of “probable adverse reaction”, providing additional weight to the causal link between tadalafil and the eruption.
Together, these frameworks transform clinical intuition into objective diagnostic confidence. In SCARs, such structured reasoning is indispensable because treatment must begin quickly—often before biopsy results return.
Histopathology: Why Biopsy Still Matters, Even When the Presentation Seems Obvious
Although AGEP can often be diagnosed clinically, histopathology remains invaluable. Classic AGEP biopsy findings include:
- subcorneal or intraepidermal pustules,
- spongiform pustules of Kogoj,
- papillary dermal edema,
- perivascular neutrophilic infiltrate,
- possible eosinophils.
The biopsy in this case conformed to the expected pattern. What biopsy more importantly did not show was keratinocyte necrosis—a hallmark of SJS/TEN. This distinction is crucial: mistaking AGEP for a necrolytic epidermal disorder could lead to unnecessary escalation, inappropriate therapies, or unwarranted concern for life-threatening progression.
Biopsy in AGEP serves two purposes: confirming the diagnosis and excluding pathologies that require very different management strategies.
Pathophysiology: Why AGEP Occurs—And Why Tadalafil Can Trigger It
AGEP is driven by a Type IVd hypersensitivity reaction, mediated by drug-specific T cells that orchestrate an exaggerated neutrophilic response. While most medications associated with AGEP are antibiotics (β-lactams, macrolides), antimalarials, calcium channel blockers, and antipyretics, the immunologic machinery does not inherently discriminate between “high-risk” and “low-risk” drugs. Any molecule capable of forming immunogenic complexes may provoke an eruption in a susceptible individual.
Tadalafil is rarely associated with SCARs, but “rare” is not synonymous with “impossible.” The mechanism may relate to:
- formation of reactive metabolites,
- neoantigen creation in hepatic metabolism,
- interaction with individual HLA profiles,
- immune activation pathways not yet characterized.
The case reinforces a key medical principle: the absence of prior association does not eliminate the possibility of hypersensitivity. Clinicians must always evaluate eruptions by their features, not by assumptions about a drug’s safety profile.
Differential Diagnosis: How AGEP Stands Apart from Its Mimics
Even an experienced clinician must pause when faced with sudden pustular eruptions. Distinguishing AGEP from its closest mimics involves a disciplined evaluation of timing, symptoms, and laboratory markers.
AGEP vs Pustular Psoriasis
The great masquerader. Pustular psoriasis is chronic, relapsing, and often involves personal or family history. Its course is slower, recurrence more likely, and systemic symptoms may be similar. Lack of a psoriatic background and rapid onset favor AGEP.
AGEP vs Stevens–Johnson Syndrome
SJS evolves over days, with mucosal ulceration, blistering, and widespread epidermal necrosis. Pustules are not a hallmark. If mucosal surfaces are spared and necrosis is absent, SJS becomes unlikely.
AGEP vs DRESS
DRESS involves prolonged latency (2–6 weeks), eosinophilia, lymphadenopathy, hepatitis, and extensive morbidity. Its presentation is more systemic and slower to resolve.
AGEP vs Acute Bacterial Infections
Follicular pustules, purulence, fever, and leukocytosis may initially suggest infection. However, AGEP pustules are sterile, nonfollicular, and accompanied by rapid desquamation.
Such differentiation determines treatment. AGEP is usually self-limited, while SJS/TEN demands intensive care and DRESS requires systemic immunosuppression. Accuracy here directly affects patient safety.
Management Strategy: Simplicity, Precision, and Avoidance of Overtreatment
AGEP is one of the few dramatic-looking dermatologic emergencies in which the treatment is deceptively gentle. Management revolves around three pillars:
1. Immediate Withdrawal of the Offending Agent
Stopping tadalafil was the turning point in this case. AGEP typically resolves within days after drug cessation, as the immune trigger dissipates.
2. Supportive Care
This includes:
- hydration,
- antipyretics,
- topical corticosteroids,
- emollients,
- antihistamines for pruritus.
Systemic corticosteroids remain controversial. Although often used, evidence suggests they do not substantially accelerate recovery. In this case, improvement occurred primarily after drug withdrawal and topical therapy.
3. Monitoring for Complications
AGEP may involve transient neutrophilia, hepatic enzyme elevation, or renal abnormalities. Although complications are generally mild compared to other SCARs, vigilance is warranted.
The patient’s favorable response underscores the benign natural course of AGEP when recognized early and treated appropriately.
Clinical Significance: Why This Case Matters More Than Its Rarity Suggests
Tadalafil’s association with AGEP may be rare, but its clinical significance is profound. PDE5 inhibitors are some of the most commonly used medications in men’s health—and increasingly in women’s and cardiovascular health. Unexpected hypersensitivity reactions, even rare ones, must be documented and understood.
This case emphasizes:
- the need for awareness of atypical drug reactions;
- the importance of structured diagnostic systems (EUROSCAR, Naranjo);
- the critical role of early recognition in minimizing morbidity;
- the caution required when prescribing even “safe” medications to individuals with extensive drug sensitivities.
For clinicians, the lesson is clear: remain vigilant but not alarmist. AGEP demands recognition, not fear. Once diagnosed correctly, it is one of the most manageable severe cutaneous reactions.
Conclusion
This case of tadalafil-induced AGEP represents a rare but instructive clinical event. The rapid onset of pustular eruption, the strong temporal relationship with drug exposure, the supportive biopsy findings, and the dramatic improvement after withdrawal all form a textbook example of AGEP.
Clinicians should remember that SCARs, while frightening in appearance, fall into distinct diagnostic patterns—and AGEP, once recognized, has an excellent prognosis. Tadalafil remains a safe drug for the vast majority of patients, but this case reminds us that pharmacologic complacency is never justified.
The real threat in AGEP is not the eruption—it is misdiagnosis. When clinicians recognize AGEP early, differentiate it accurately, and treat it conservatively but attentively, patients recover completely and rapidly.
FAQ
1. Can tadalafil truly cause AGEP, or was this an isolated coincidence?
Yes, tadalafil can trigger AGEP, as demonstrated by EUROSCAR and Naranjo scoring. The reaction is rare but mechanistically plausible.
2. Does AGEP require systemic corticosteroids?
Not necessarily. Most patients recover with drug withdrawal, topical therapy, and supportive care. Steroids may be used in selected severe cases but are not mandatory.
3. Should patients who develop AGEP avoid all PDE5 inhibitors?
Cross-reactivity is unlikely but cannot be ruled out. A thorough allergy evaluation is recommended, and alternative therapies may be considered depending on clinical need.