Introduction
Erectile dysfunction (ED) is defined as the persistent inability to achieve and maintain an erection sufficient for satisfactory sexual performance. Far from being a trivial inconvenience, ED is a condition with broad implications for physical, psychological, and relational health. Current global estimates suggest that over 320 million men may be affected by ED by 2025, with prevalence varying between 15% and 60% depending on geography, comorbidities, and age distribution.
The introduction of oral phosphodiesterase type 5 inhibitors (PDE5i) revolutionized ED management. Since the late 1990s, sildenafil, tadalafil, vardenafil, and more recently avanafil have become first-line therapies. These agents share a common mechanism—blocking PDE5 and thereby increasing cyclic guanosine monophosphate (cGMP), enhancing nitric oxide–mediated vasodilation in penile tissue.
But clinical practice is rarely just about mechanisms. It is about preferences, persistence, satisfaction, side effects, and lived experience. Among PDE5i, sildenafil (Viagra®) and tadalafil (Cialis®) dominate prescriptions. Both are effective, but differences in pharmacokinetics, side-effect profiles, and patient-reported outcomes have long fueled debate: which is the superior choice?
The systematic review and meta-analysis by Gong et al. (2017) provided a direct comparison across 16 clinical trials involving over 5,000 patients. Their analysis offers rare clarity on a question clinicians face daily. Let us dissect the findings and their implications.
Efficacy: Do Sildenafil and Tadalafil Work Equally Well?
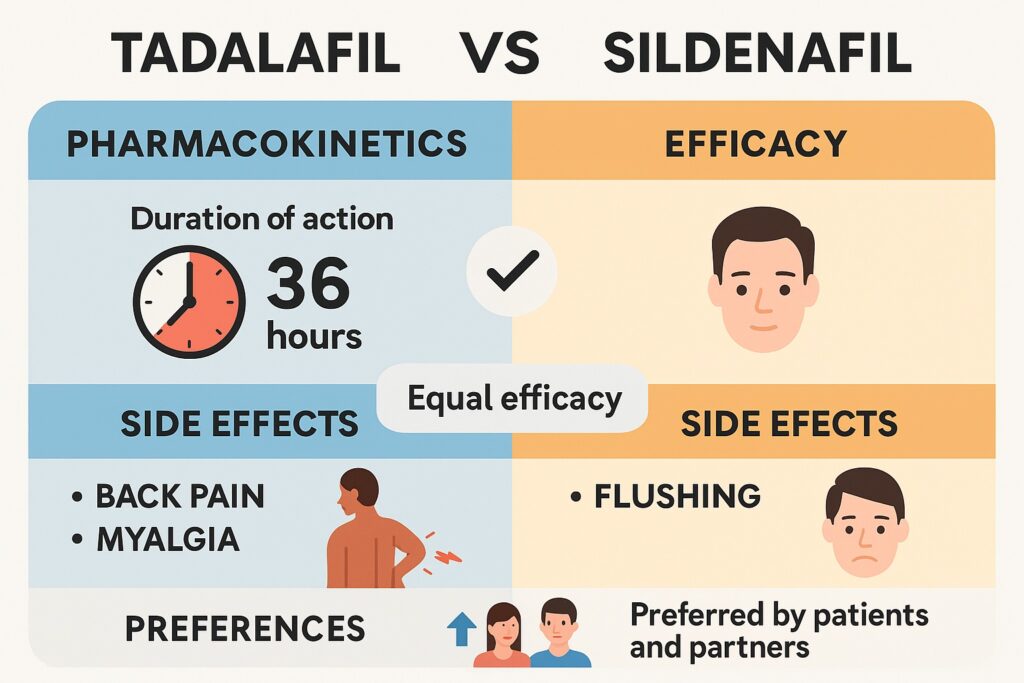
When it comes to the primary goal—erection quality—both drugs perform admirably and, importantly, comparably. Across studies, there was no significant difference between sildenafil and tadalafil in improving scores on the International Index of Erectile Function (IIEF-EF).
Intercourse satisfaction, sexual desire, and overall satisfaction domains also showed no statistically significant differences. This result may surprise some clinicians who believe in the clinical folklore that “tadalafil works longer, sildenafil works stronger.” The evidence suggests efficacy is not a matter of superiority but equivalence.
Still, the absence of difference in raw erectile outcomes does not imply the drugs are interchangeable. Patients value more than penile rigidity—they value control, confidence, and spontaneity. This is where nuances emerge.
Psychological Outcomes: The Hidden Strength of Tadalafil
ED is rarely just a vascular problem. The psychological burden—anxiety, fear of failure, loss of confidence—often eclipses the mechanical deficit. Treatment, therefore, should aim not only to restore erections but also to restore dignity and self-assurance.
The meta-analysis found tadalafil significantly outperformed sildenafil in psychosocial measures:
- SEAR Confidence Scores: Patients on tadalafil reported greater improvements in sexual self-confidence.
- SEAR Sexual Relationship Scores: Couples reported better relational outcomes with tadalafil.
- EDITS (Erectile Dysfunction Inventory of Treatment Satisfaction): Tadalafil users showed higher overall satisfaction scores.
Why this difference? Pharmacokinetics offers part of the answer. Tadalafil’s half-life of 17.5 hours allows efficacy up to 36 hours, compared with sildenafil’s 4-hour half-life. This “weekend pill” effect liberates couples from the tyranny of scheduling intimacy around medication. The ability to “be ready anytime” translates into reduced performance anxiety and improved confidence.
Thus, while raw efficacy may be equal, tadalafil wins in the psychological arena, which is arguably just as important.
Patient and Partner Preference: Votes with Action
Nine studies included direct data on men’s treatment preferences, and two assessed partner preferences. The pooled results are striking:
- Men were 8 times more likely to prefer tadalafil over sildenafil.
- Women were even more decisive, being 14 times more likely to prefer tadalafil for their partner.
Why such a strong tilt toward tadalafil? Likely explanations include:
- Longer duration of action allowing spontaneity
- Less planning stress during sexual encounters
- Improved relational confidence as reflected in SEAR and EDITS scores
This preference data underscores a fundamental truth in sexual medicine: patient-centered outcomes matter more than clinician assumptions.
Adherence and Persistence: Do Patients Stick with Therapy?
Drug efficacy in trials is one thing; adherence in real life is another. Discontinuation rates for PDE5 inhibitors remain surprisingly high, with up to 50% of patients abandoning therapy within two years. Reasons include dissatisfaction, adverse effects, cost, or relational factors.
The meta-analysis revealed no significant difference between tadalafil and sildenafil in adherence or persistence at three and six months. This finding suggests that while patients may prefer tadalafil, real-world continuation rates are influenced by broader psychosocial and economic factors rather than pharmacology alone.
Safety Profiles: Similar Overall, but Different Flavors
Both sildenafil and tadalafil share overall similar rates of adverse events, with no statistically significant difference in total side-effect incidence. However, their profiles diverge in detail:
- Tadalafil was associated with higher rates of myalgia and back pain. These are thought to stem from PDE11 cross-inhibition in skeletal muscle.
- Sildenafil had higher rates of flushing due to stronger vasodilatory effects on peripheral vessels.
- Incidences of headache, dyspepsia, nasal congestion, and nasopharyngitis were comparable.
The key takeaway is that neither drug is riskier overall, but side effects differ qualitatively. Clinicians should tailor therapy based on patient tolerance: men with prior musculoskeletal complaints may favor sildenafil, while those prone to flushing may prefer tadalafil.
The Pharmacokinetic Divide: Timing Is Everything
Beyond efficacy and safety, pharmacokinetics shape patient experience.
- Sildenafil: Onset ~30 minutes; duration 4–6 hours; effective window up to 12 hours. Best suited for planned encounters.
- Tadalafil: Onset ~20–30 minutes; duration up to 36 hours. Effective in 50% of men within 30 minutes. Allows spontaneity across multiple attempts.
This distinction fuels preference. For couples seeking planned intimacy, sildenafil suffices. For those who prioritize flexibility and reduced time pressure, tadalafil is the clear winner.
Limitations of the Evidence
The meta-analysis is robust but not flawless. Limitations include:
- Heterogeneity across studies in dosing regimens and study designs.
- Variable quality of included trials, with many being open-label rather than double-blind.
- Publication bias detected in certain adverse event outcomes (e.g., flushing, headache).
- Short-term follow-up, with most studies spanning only a few months.
These constraints temper certainty but do not negate the overall conclusions.
Clinical Implications: Choosing Between Two Equals
So, how should a clinician decide between sildenafil and tadalafil? The evidence suggests:
- Efficacy is equal: Both reliably restore erectile function.
- Safety is equal overall, but side-effect flavors differ.
- Preference leans heavily toward tadalafil, particularly among partners.
- Psychological outcomes favor tadalafil, thanks to reduced time pressure and increased confidence.
In short, tadalafil may be the better first-line option, not because it creates stronger erections, but because it creates stronger relationships.
Conclusion
This systematic review and meta-analysis provides one of the clearest direct comparisons between tadalafil and sildenafil. Both are effective and safe for erectile dysfunction, with no major differences in raw erectile outcomes. Yet the longer half-life of tadalafil, combined with its superior impact on psychological outcomes and overwhelming patient preference, tips the scales in its favor.
ED therapy is not about pharmacology in isolation—it is about restoring intimacy, confidence, and quality of life. In this broader context, tadalafil emerges not only as a drug of choice but as a relationship enhancer. Sildenafil remains a valuable tool, but tadalafil may simply fit better into the rhythms of modern life.
FAQ
1. Is tadalafil truly more effective than sildenafil?
Not in terms of raw erection quality—both are equally effective. The main difference lies in psychological outcomes and patient preference, where tadalafil excels.
2. Why do more patients and partners prefer tadalafil?
Because tadalafil lasts up to 36 hours, it reduces the need for planning, alleviates performance anxiety, and increases confidence, leading to higher satisfaction for both men and their partners.
3. What about side effects—should patients worry?
Both drugs are safe overall. Tadalafil may cause more back pain and myalgia, while sildenafil more often causes flushing. Choice should be individualized based on tolerance.