Introduction
Erectile dysfunction (ED) is not simply a disorder of intimacy—it is a vascular and systemic signal often marching in step with hypertension, diabetes, hyperlipidemia, and obesity. Both ED and hypertension share a common denominator: endothelial dysfunction and impaired vascular regulation. Not surprisingly, men with hypertension are significantly more likely to develop ED, and in some cases, ED precedes overt cardiovascular disease by several years.
The widespread use of phosphodiesterase type 5 inhibitors (PDE5i) such as tadalafil has transformed ED management. However, the clinical question remains: can these vasodilators safely coexist with antihypertensive therapy, or do they pose a risk of hypotension and adverse cardiovascular outcomes? While controlled trials suggest modest blood pressure reductions, the true safety profile in the real world, where multimorbidity and polypharmacy reign, has been less clear.
A large retrospective observational study using U.S. electronic health records sought to answer this question. The findings challenge long-standing cautionary tales and provide reassurance for clinicians navigating the overlapping terrain of cardiovascular and sexual health.
The Intersection of Hypertension and Erectile Dysfunction
Hypertension is the world’s leading cause of mortality, accounting for over 10 million deaths annually. In the United States, nearly half of adults have either a diagnosis of hypertension or are on antihypertensive therapy. ED, meanwhile, affects 18.4% of men over 20 years, with prevalence increasing sharply with age—ranging from 5% in younger men to over 70% in men over 70.
The two conditions often overlap:
- Up to 41.6% of men with ED also have hypertension.
- Men with ED are 38% more likely to be hypertensive compared with those without ED.
- Certain antihypertensive drugs—particularly thiazide diuretics and beta-blockers—may themselves worsen erectile function, contributing to poor adherence.
Thus, men with ED frequently present a therapeutic paradox: medications essential for cardiovascular survival may compromise sexual quality of life. This reality drives some men to discontinue antihypertensives without medical guidance, undermining blood pressure control and increasing long-term cardiovascular risk.
Pharmacological Concerns: PDE5 Inhibitors and Blood Pressure
Tadalafil and other PDE5 inhibitors function as vasodilators, enhancing the nitric oxide–cGMP pathway. While this mechanism improves penile blood flow, it may also lower systemic blood pressure.
Guidelines outline specific cautions:
- Contraindication with nitrates and riociguat due to profound hypotensive risk.
- Caution with alpha-blockers, where additive vasodilation may precipitate symptomatic hypotension.
- Relative safety with standard antihypertensives (thiazides, calcium channel blockers, ACE inhibitors, ARBs, beta-blockers), though labeling advises vigilance.
Clinical pharmacology trials report only modest, transient reductions in blood pressure when PDE5 inhibitors are combined with antihypertensives. Yet, uncertainty has lingered: do these mild changes translate into meaningful risks of syncope, arrhythmia, myocardial infarction, or stroke in the real world?
Study Design: Real-World Data at Scale
To address this, researchers harnessed the Optum EHR Research Database, encompassing data from over 92,000 providers and 195 hospitals across the U.S. The study spanned 2012 to 2017, identifying men prescribed tadalafil and/or antihypertensive medications.
Key features:
- Population: 360,154 men with ED and eligible prescriptions.
- Exposure cohorts:
- Tadalafil + antihypertensive (127,849 possession periods)
- Antihypertensive only (821,359 possession periods)
- Tadalafil only (98,638 possession periods)
- Exclusions: use of nitrates, riociguat, alpha-blockers.
- Matching: Propensity score techniques ensured comparability across cohorts.
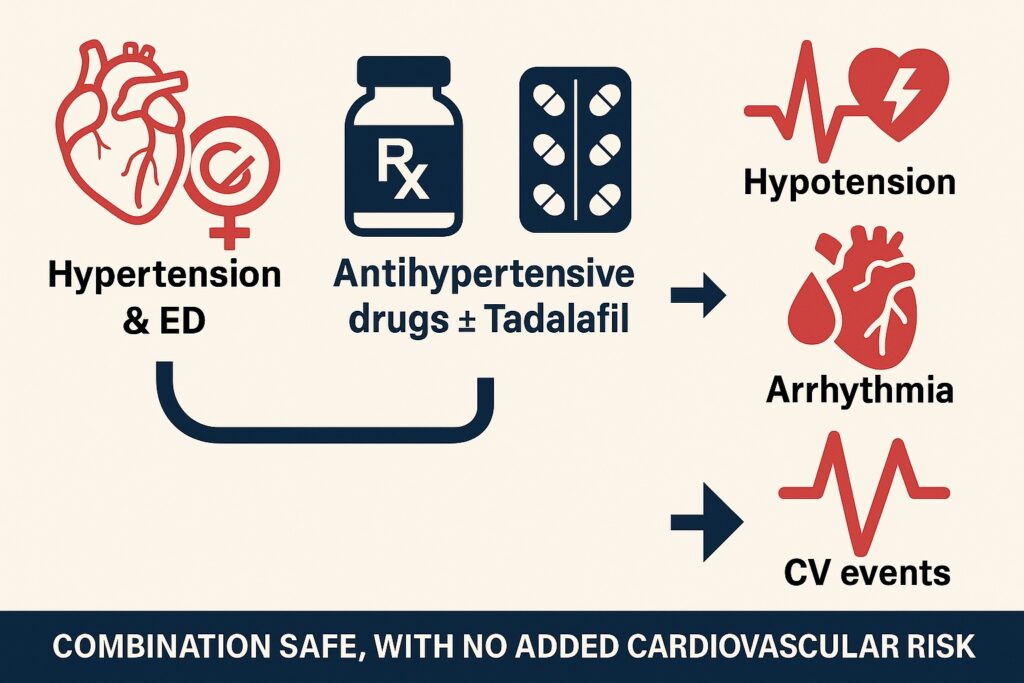
- Outcomes: Hypotension, syncope, arrhythmia, myocardial infarction, stroke, heart failure, cardiovascular death, all-cause death.
Importantly, the study examined possession periods—time frames when patients were likely to have medication available, acknowledging that actual adherence may vary.
Results: Safety Signals or Reassurance?
The findings were both surprising and reassuring.
- Hypotension: No increased risk. In fact, the incidence of diagnosed hypotension was lower in the tadalafil + antihypertensive group compared to antihypertensive-only patients (IRR 0.79; 95% CI 0.71–0.89).
- Arrhythmia: Ventricular arrhythmia risk was modestly lower with tadalafil co-possession (IRR 0.79; 95% CI 0.66–0.94).
- All-cause mortality: Strikingly, the risk was reduced (IRR 0.55; 95% CI 0.36–0.86).
- Cardiovascular death: No significant increase; effect neutral.
- Other cardiovascular outcomes (myocardial infarction, stroke, syncope, hospitalization for heart failure): No significant risk elevation.
Even natural language processing of free-text clinical notes—capturing softer outcomes like dizziness—revealed no concerning trends.
Interpretation: Why the Reduced Risks?
The absence of increased risk—and the suggestion of reduced mortality—invites several interpretations:
- Selection bias: Physicians may preferentially prescribe tadalafil to healthier hypertensive patients, inadvertently skewing results toward better outcomes.
- Vascular benefits of PDE5 inhibitors: Beyond erectile tissue, PDE5i improve endothelial function, increase arterial compliance, and may exert cardioprotective effects.
- Improved adherence: Treating ED may motivate men to remain adherent to antihypertensive therapy, indirectly improving blood pressure control.
Thus, what was once feared as a dangerous combination may, under proper supervision, represent a synergistic therapeutic strategy.
Clinical Implications
This study shifts the clinical conversation. Physicians often hesitate to prescribe tadalafil to men on antihypertensives, fearing catastrophic hypotension. These real-world data suggest such fears may be exaggerated.
Practical takeaways:
- Safe to prescribe tadalafil alongside standard antihypertensives, provided contraindications (nitrates, riociguat, cautious alpha-blocker use) are respected.
- Patient counseling remains essential: inform patients about the possibility of mild dizziness or blood pressure changes, but reassure them about the low likelihood of serious events.
- Do not withhold therapy: denying ED treatment in hypertensive men may worsen adherence to blood pressure medications, undermining cardiovascular outcomes.
Limitations of the Evidence
No study is perfect, and this one is no exception:
- Retrospective design: confounding by indication remains possible.
- Medication possession ≠ medication use: adherence cannot be guaranteed.
- Residual bias: unmeasured variables (severity of hypertension, sexual activity, lifestyle) may distort associations.
- Excluded alpha-blockers and nitrates: results cannot be extrapolated to these high-risk groups.
Nonetheless, the study’s sheer scale, use of propensity matching, and innovative integration of natural language processing strengthen its credibility.
Conclusion
In the largest real-world assessment to date, co-possession of tadalafil and antihypertensive medications was not associated with increased risk of hypotensive or cardiovascular outcomes. On the contrary, certain outcomes—including hypotension, arrhythmia, and all-cause mortality—were less frequent among co-users.
For clinicians, the message is clear: tadalafil can be safely prescribed in hypertensive men with ED, provided standard contraindications are respected. For patients, the findings reinforce that treating ED need not come at the expense of cardiovascular safety—and may, in fact, enhance overall health outcomes.
FAQ
1. Can men on blood pressure medications safely take tadalafil?
Yes, provided they are not on nitrates or riociguat. Real-world data show no increased risk of hypotension or cardiovascular events.
2. Does tadalafil lower blood pressure dangerously when combined with antihypertensives?
No. While tadalafil causes mild vasodilation, studies show only modest, clinically insignificant reductions in blood pressure when combined with standard antihypertensives.
3. Could tadalafil actually benefit cardiovascular health?
Possibly. By improving endothelial function and encouraging adherence to antihypertensive therapy, tadalafil may indirectly reduce cardiovascular risks, though more prospective data are needed.