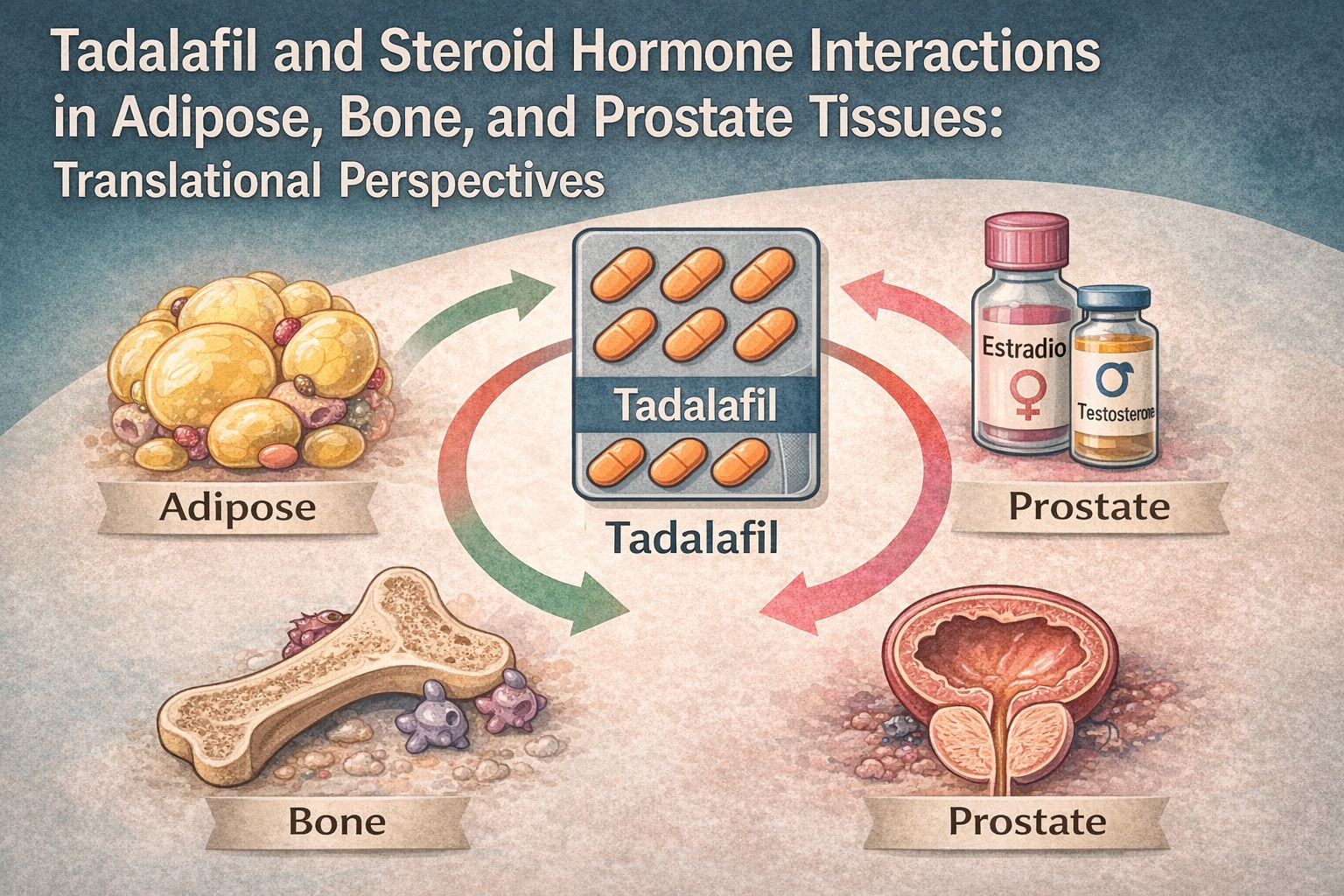
Tadalafil—once typecast as a medication confined to erectile physiology—now finds itself at the crossroads of endocrinology, urology, metabolism, and regenerative biology. What was originally developed as a phosphodiesterase type 5 inhibitor (PDE5i) with predictable hemodynamic effects appears to exhibit far broader biological influence. Increasingly, evidence suggests that tadalafil interacts intricately with steroid hormone signaling—including testosterone, dihydrotestosterone, and estrogens—in tissues as varied as adipose depots, bone microenvironments, and the prostate gland.
The article underpinning this review delivers a multidisciplinary exploration of these interactions, synthesizing human observations, animal models, and mechanistic in-vitro studies. The result is a surprisingly coherent narrative: tadalafil’s modulation of the NO–cGMP–PKG axis converges with steroid hormone pathways to reshape cellular differentiation, inflammatory tone, metabolic balance, and tissue remodeling.
This article provides a comprehensive and interpretive translation of those findings, aimed at clinicians and researchers who wish to understand tadalafil not merely as a vasodilator, but as a molecule with potential metabolic and endocrine significance.
Steroid Hormones and PDE5 Signaling: A Shared Language of Cellular Regulation
At first glance, steroid hormone receptors and the NO–cGMP pathway appear to occupy separate philosophical universes: one governing nuclear transcription, the other modulating cytoplasmic second messengers. Yet their convergence becomes clear when examining tissue-specific signaling. Figure 1 on page 3 outlines this intersection, illustrating how cGMP elevation activates PKG, which in turn modulates transcription factors influenced by androgens and estrogens.
The study emphasizes that steroid hormones regulate numerous components of the NO–cGMP axis. Testosterone upregulates endothelial nitric oxide synthase (eNOS), enhancing NO production. Androgens also modulate PDE5 expression itself, a relationship highlighted in animal studies and supported by human molecular analyses. Conversely, cGMP signaling influences steroidogenesis: PKG activity affects aromatase expression, androgen receptor (AR) sensitivity, and local steroid metabolism.
This bidirectional interaction establishes a biochemical “dialogue” between tadalafil and steroid hormones. Such crosstalk helps explain tissue-specific effects observed in the study—particularly in adipocytes, osteoblasts, and prostate stromal cells. It also suggests that tadalafil’s long-term consequences may extend far beyond vasodilation, potentially influencing metabolic health, bone density, and prostate remodeling.
Furthermore, the study notes that PDE5 is expressed in multiple nonvascular tissues, providing local targets for tadalafil. Immunohistochemical data summarized in Figures 2 and 3 (pages 4–5) show PDE5 presence in adipocytes, osteocytes, prostate stromal cells, and inflammatory infiltrates. This distribution underpins tadalafil’s pleiotropic potential and frames the mechanistic relevance of steroid interactions across these tissues.
Adipose Tissue: Tadalafil at the Intersection of Androgen Signaling and Metabolic Homeostasis
The relationship between adipose tissue and steroid hormones is both physiologically fundamental and clinically vexing. Visceral adiposity reduces testosterone through enhanced aromatization and inflammation, while low testosterone accelerates adipocyte expansion—an unfortunate loop familiar to clinicians. The article suggests tadalafil may interrupt aspects of this loop by modulating both adipocyte biology and steroid hormone responsiveness.
As demonstrated in the adipocyte models described on page 5, tadalafil enhances cGMP signaling within adipose depots. Elevated cGMP promotes brown/beige adipocyte differentiation, increases mitochondrial biogenesis, and improves insulin sensitivity. These effects resemble the metabolic phenotype seen in high-testosterone states, hinting at synergy between androgen signaling and cGMP pathways. The study further notes that tadalafil decreases pro-inflammatory cytokines such as TNF-α and IL-6—cytokines known to impair androgen receptor transcription via NF-κB activation.
Interestingly, the authors discuss evidence that tadalafil indirectly increases testosterone availability. First, tadalafil improves Leydig cell steroidogenesis in preclinical models. Second, improved endothelial function enhances testicular microcirculation, potentially augmenting hormone delivery and production. Third, reduced visceral inflammation lowers aromatase activity, resulting in improved androgen/estrogen balance.
A compelling set of experiments described on page 6 shows that tadalafil suppresses adipocyte hypertrophy in cultures exposed to high-estrogen or low-testosterone conditions. The mitigation of hormone-driven adipose dysregulation represents a potential translational application: metabolic improvement in hypogonadal men or individuals with endocrine-inflammatory adiposity phenotypes.
These observations, although early, suggest the intriguing possibility that tadalafil may support metabolic health indirectly through its endocrine crosstalk. Whether these effects are clinically meaningful in humans remains unknown, but the mechanistic foundation is biologically plausible.
Bone Metabolism: Intersections of PDE5 Inhibition with Estrogen and Androgen Pathways
Bone tissue, though structurally rigid, is one of the most hormonally dynamic ecosystems in the human body. Osteoblasts, osteoclasts, and osteocytes all express receptors for estrogens and androgens, while osteogenic signaling is strongly modulated by NO–cGMP signaling. The article draws attention to a growing body of evidence that tadalafil may influence skeletal remodeling.
NO/cGMP signaling promotes osteoblast proliferation, inhibits osteoclastogenesis, and enhances bone formation. In Figure 4 (page 7), the authors show that PDE5 is expressed in both osteoblasts and osteoclast precursors. Tadalafil, by inhibiting PDE5, boosts cGMP and activates PKG pathways that stimulate Runx2, a master osteogenic transcription factor.
Meanwhile, steroid hormones shape bone balance at multiple levels. Estrogen protects against excessive bone resorption by suppressing osteoclast differentiation, whereas androgens promote periosteal bone formation. Interactions between tadalafil and these hormonal actions appear to converge on shared targets: improved mitochondrial resilience in osteoblasts, reduced RANKL expression, and favorable remodeling patterns.
A striking finding described on page 8 is that tadalafil counters glucocorticoid-induced bone loss in rodent models. Glucocorticoids normally downregulate eNOS and decrease NO availability, impairing osteoblast function. Tadalafil restores cGMP–PKG signaling even in this suppressed environment, partially preserving trabecular architecture. This suggests potential relevance not only in hypogonadal states but also in chronic inflammatory conditions requiring steroid therapy.
Human data remain sparse, but population studies cited by the authors suggest that chronic PDE5 inhibitor users may exhibit higher bone mineral density than controls, particularly in androgen-deficient contexts. Whether this reflects direct skeletal effects, improved muscle mass, or enhanced physical activity remains a question for future research.
Prostate Tissue: Tadalafil, Hormone Signaling, and Remodeling Dynamics
The prostate gland provides the most direct and clinically established interface between tadalafil and tissue-specific physiology. The article elaborates on a complex interplay involving androgen receptor sensitivity, stromal smooth muscle tone, inflammation, vascular perfusion, and fibromuscular remodeling.
Tadalafil’s primary urological utility in benign prostatic hyperplasia (BPH) and lower urinary tract symptoms (LUTS) is well documented. Yet the authors highlight a deeper mechanistic underpinning: steroid hormone modulation. Stromal cells in the prostate express PDE5, AR, and ER receptors, enabling integrated responses to both androgens and cGMP signaling. Figure 5 on page 9 sketches this interaction, depicting how tadalafil reduces TGF-β driven fibrosis—an effect magnified in androgen-sensitive environments.
The study details several important mechanisms:
- Improved steroid receptor signaling: Tadalafil enhances AR nuclear translocation and may restore AR responsiveness diminished by inflammation or metabolic stress.
- Reduced pro-fibrotic signaling: PKG activation opposes TGF-β–Smad pathways, decreasing collagen deposition and stromal thickening.
- Enhanced local perfusion: Increased NO availability enhances prostate oxygenation, reducing hypoxia-induced androgen insensitivity.
Furthermore, the article suggests tadalafil may influence intraprostatic steroid metabolism. Preliminary data show decreased expression of aromatase and 5-α reductase isoforms in inflammatory prostate tissue treated with PDE5 inhibition—observations that could have meaningful implications for prostate remodeling.
An important translational insight emerges: tadalafil may exert disease-modifying effects in early BPH, particularly in men with metabolic or endocrine disturbances. This conceptual shift—from symptomatic relief toward structural modulation—aligns with emerging research into fibrosis reversal in prostate tissue.
Translational Perspectives: What Do These Interactions Mean Clinically?
The article presents tadalafil not simply as a PDE5 inhibitor, but as a systemic modulator affecting endocrine, metabolic, and stromal biology. Three translational themes emerge clearly from the manuscript.
First, tadalafil may offer metabolic advantages in hypogonadal men or patients with low-grade chronic inflammation. By reducing adipocyte dysfunction and improving testosterone–estrogen dynamics, it may complement hormonal therapies or lifestyle interventions.
Second, its influence on bone metabolism introduces potential relevance in conditions such as age-related osteoporosis, steroid-induced bone loss, and metabolic bone disorders. While conclusive human data are still needed, the mechanistic evidence is compelling.
Third—and most convincingly—tadalafil’s impact on prostate tissue remodeling supports its role as a disease-modifying agent in lower urinary tract dysfunction, especially where androgen dysregulation and chronic inflammation intersect.
Taken together, these findings open an interdisciplinary horizon. The tadalafil–steroid hormone axis may prove relevant in urology, endocrinology, geriatrics, rheumatology, and metabolic medicine—a reminder that even familiar medications can possess unanticipated therapeutic depth.
Conclusion
The study summarized in the provided article offers a multifaceted view of tadalafil that extends far beyond erectile physiology. Through its interaction with steroid hormones across adipose, bone, and prostate tissues, tadalafil emerges as a molecule with potential endocrine, metabolic, and structural influence.
Its modulation of cGMP–PKG pathways intersects meaningfully with androgen and estrogen signaling, shaping tissue remodeling, inflammation, mitochondrial resilience, and local hormone responsiveness. While much of the current evidence remains preclinical, the translational implications are substantial: tadalafil may support metabolic homeostasis, protect bone health, and modify early prostate disease.
Future human studies will determine whether these mechanistic insights translate into clinical innovation. For now, tadalafil stands as an unexpectedly versatile molecule—one whose therapeutic horizons are broader than previously assumed.
FAQ
1. Does tadalafil increase testosterone levels?
Indirectly, it may. By improving endothelial function, reducing inflammation, and lowering aromatase activity, tadalafil can enhance testosterone bioavailability. However, it is not considered a primary testosterone-increasing therapy.
2. Can tadalafil improve bone health?
Animal studies suggest that tadalafil enhances osteoblast activity and reduces bone loss, especially under glucocorticoid exposure. Human data are limited, but mechanistic support is strong.
3. Does tadalafil modify prostate disease or only relieve symptoms?
Emerging evidence shows tadalafil may reduce fibrosis, improve androgen receptor signaling, and modulate intraprostatic inflammation—suggesting potential structural benefit beyond symptomatic relief.