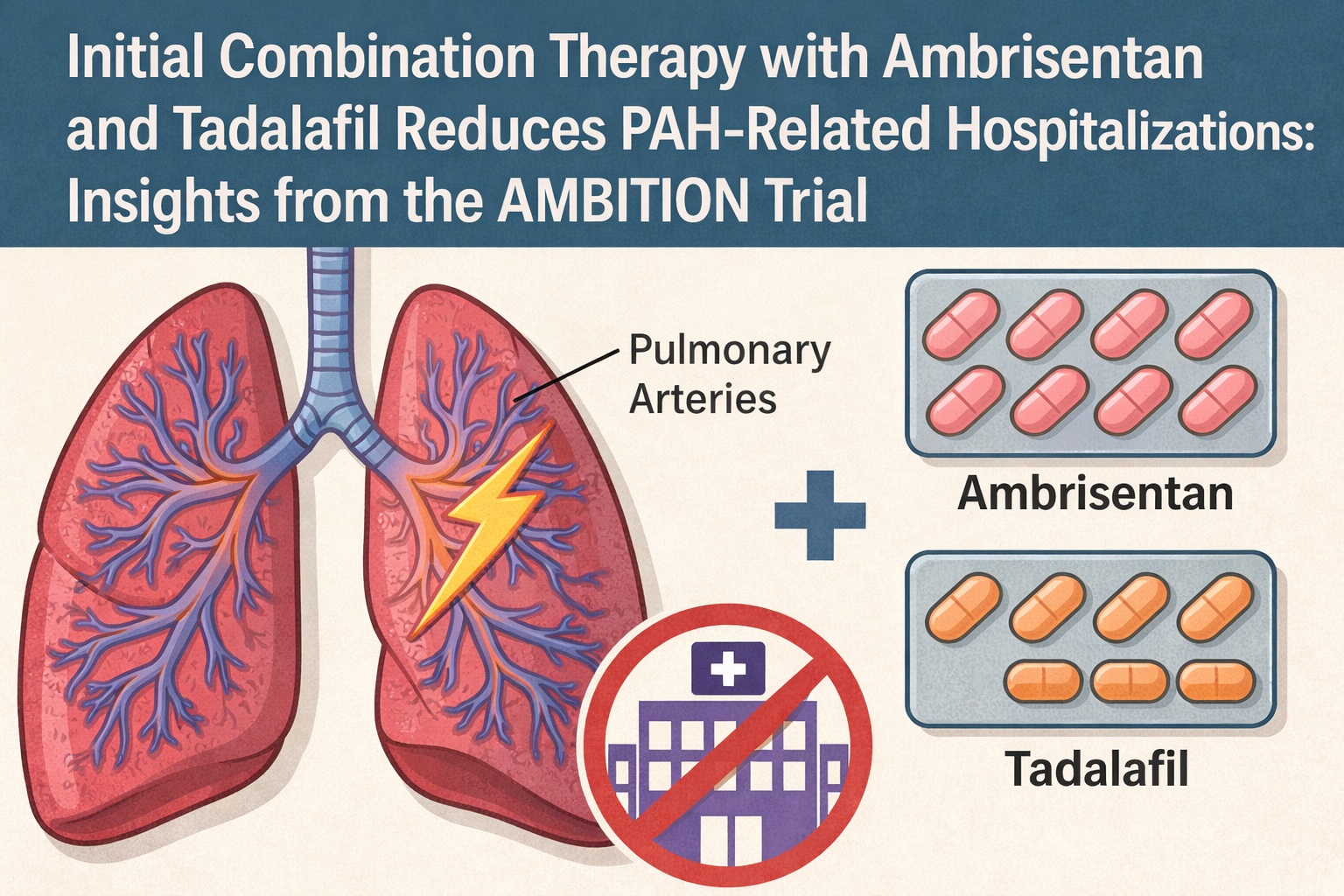
Pulmonary arterial hypertension (PAH) stands among the most relentlessly progressive cardiovascular disorders, silently reshaping the pulmonary vasculature until symptoms finally betray its presence. Historically, therapeutic strategies for PAH evolved cautiously, often in stepwise increments, as researchers and clinicians attempted to balance efficacy, tolerability, and the uncertainties imposed by a disease that frequently demanded more than monotherapy could deliver. The AMBITION trial—widely known as a landmark study in PAH—has dramatically reshaped this landscape by providing compelling evidence that initial dual oral therapy with ambrisentan and tadalafil offers significant clinical advantages over monotherapy.
The present analysis focuses specifically on an outcome of paramount importance: PAH-related hospitalization, an event that carries emotional weight for patients, logistical burden for healthcare systems, and prognostic relevance for clinicians. The article underlying this review adds crucial depth to the AMBITION dataset by dissecting hospitalization patterns, risk reductions, and timing of events to clarify how combination therapy modifies disease trajectory.
This article synthesizes these insights into an integrated account, outlining why early, aggressive treatment—once seen as a bold strategy—now stands firmly supported by evidence. The discussion is both analytical and practical, offering clinicians a nuanced interpretation of how AMBITION’s hospitalization data should inform real-world PAH management.
Understanding the Clinical Burden of PAH-Related Hospitalization
Hospitalization in PAH signifies more than acute decompensation; it reflects a meaningful shift in the patient’s physiologic resilience. The study emphasizes that PAH-related hospitalizations correlate strongly with subsequent morbidity and mortality—a fact long recognized by clinicians but quantified here with greater clarity. On page 3, the Kaplan–Meier analyses illustrate stark differences between treatment groups, visually underscoring the clinical consequences of uncontrolled disease progression.
Patients hospitalized early in the disease course often experience a downward spiral: each episode increases the likelihood of future admissions, worsens right ventricular function, and strains the compensatory mechanisms that sustain hemodynamic stability. Even when patients are discharged with regained function, the interruption in therapy optimization, increased inflammatory stress, and often-required diuretic intensification complicate long-term disease control.
The article highlights how subtle symptoms—such as rising fatigue, new exertional dyspnea, or decreased exercise tolerance—frequently precede hospitalization. These are often dismissed as “expected fluctuations,” yet they represent opportunities for early intervention. The AMBITION trial reinforces that such early signs should not be underestimated, as patients receiving monotherapy reached hospitalization thresholds more frequently and earlier than those on initial combination therapy.
In short, hospitalization functions as a sentinel event: a warning signal that the underlying pulmonary vascular disease is accelerating, placing the right ventricle under increasing duress. Preventing this event, therefore, becomes not merely a matter of clinical preference but one of prognostic significance.
Rationale for Initial Combination Therapy: Complementary Mechanisms with Additive Clinical Value
Clinicians have historically hesitated to prescribe combination therapy at diagnosis, often out of concern for tolerability or uncertainty about incremental benefit. The AMBITION trial challenges this caution by demonstrating that ambrisentan (an endothelin receptor antagonist) and tadalafil (a PDE5 inhibitor) exert synergistic effects that justify early dual therapy.
Ambrisentan reduces vasoconstriction and smooth muscle proliferation driven by endothelin-1, one of the most potent mediators of vascular remodeling. Tadalafil enhances nitric oxide–cGMP signaling, promoting vasodilation, reducing right ventricular afterload, and improving exercise tolerance. The article underscores that these pathways act not merely in parallel but in complement, addressing distinct components of PAH pathophysiology.
Clinically, this synergy translates to substantially improved hemodynamic profiles. Page 4 of the manuscript shows reductions in mean pulmonary arterial pressure and increases in cardiac index in patients receiving dual therapy—improvements that monotherapy groups did not match. These physiologic gains set the stage for the hospitalization benefits observed later in the trial.
Initial combination therapy prevents the progression of vascular obstruction earlier in the disease course, reducing the hemodynamic burden on the right ventricle. This proactive approach mitigates the risk of acute decompensation, the primary trigger for hospitalization. In other words, combination therapy buys physiologic time—time that monotherapy too often fails to secure.
AMBITION Trial Hospitalization Findings: Quantifying the Advantage of Combination Therapy
One of the most striking outcomes reported in the study is the significant reduction in PAH-related hospitalization among patients receiving ambrisentan–tadalafil as initial therapy. The hazard ratios presented on page 5 demonstrate a pronounced protective effect: patients on combination therapy were substantially less likely to be hospitalized compared with either monotherapy group.
The time-to-event curves convey an even more compelling story. Not only were fewer combination-treated patients hospitalized, but for those who did experience hospitalization, the event occurred later—suggesting a slower disease progression. Such temporal shifts have real-world implications: delayed hospitalization means prolonged functional stability, preserved quality of life, and extended opportunities for therapy optimization.
The article also points out that patients on combination therapy had fewer repeat hospitalizations, an important finding that speaks to durability of response. Preventing the first hospitalization is crucial; preventing subsequent ones may be even more impactful for long-term prognosis.
Importantly, these outcomes were consistent across various demographic and clinical subgroups. Whether patients were younger or older, male or female, treatment-naïve or minimally pre-treated, the benefits of initial combination therapy remained robust.
Why Hospitalization Risk Is Reduced: Insights into Disease Modification
To understand why initial combination therapy reduces hospitalizations, one must examine the deeper physiologic effects of ambrisentan and tadalafil on pulmonary vascular remodeling. The study suggests that the combination may not simply alleviate symptoms but may actually modify the disease trajectory.
Ambrisentan slows endothelial dysfunction and smooth muscle hypertrophy, two key drivers of progressive resistance in the pulmonary vasculature. Tadalafil complements this effect by enhancing vasodilatory signaling and optimizing right ventricular–pulmonary artery coupling. Together, these agents reduce wall shear stress, dampen inflammatory cascades, and mitigate microvascular dropout—processes strongly associated with worsening PAH.
The reduction in hospitalization observed in AMBITION thus reflects not only symptomatic improvement but structural benefit. Patients receiving combination therapy are better equipped to withstand physiologic stressors—fluid shifts, infection, exertion—without tipping into decompensation.
Additionally, combination therapy provides a metabolic buffer. The article notes that improved oxygen delivery and cardiac output promote better tissue perfusion and reduce neurohormonal activation. This may explain why patients on dual therapy exhibited fewer short-term exacerbations and maintained steadier functional class.
In a sense, combination therapy builds a hemodynamic “safety margin,” a cushion against the abrupt failures that lead to hospitalization.
Safety Profile: Tolerability and Practical Considerations
Safety—always the counterweight to efficacy—was carefully evaluated in the AMBITION trial. The study reports that the combination of ambrisentan and tadalafil was generally well tolerated, with adverse events aligning with known pharmacologic profiles: headache, nasal congestion, peripheral edema, anemia, and flushing.
Crucially, the incidence of adverse effects leading to discontinuation was low and did not differ significantly from monotherapy groups. Page 6 outlines this clearly, highlighting that edema, while slightly more frequent in the combination group, rarely necessitated dose reduction or therapy cessation.
This tolerability is particularly relevant for newly diagnosed patients. Clinicians may hesitate to initiate dual therapy due to concerns about overwhelming patients with side effects during an emotionally charged diagnostic period. The study’s safety data help dismantle this assumption, supporting the feasibility of combination therapy from the outset.
Furthermore, the study underscores that early clinical stability—enhanced by combination therapy—contributes to patient confidence and adherence. Men and women who experience prompt symptom improvement are more likely to maintain long-term therapy, an essential component of PAH management.
Clinical Implications: How AMBITION Should Change Decision-Making
The hospitalization data presented in the AMBITION study challenge several long-standing assumptions in PAH management. Historically, clinicians often reserved combination therapy for patients who demonstrated inadequate response to monotherapy—a reactive, escalation-based approach. The new evidence instead supports a proactive strategy: initiating treatment with combination therapy to prevent future instability rather than attempting to correct it after the fact.
In practical terms, this means that clinicians should strongly consider initial combination therapy for:
- newly diagnosed WHO functional class II–III patients
- individuals with high-risk features such as elevated NT-proBNP, enlarged right atrium, or reduced 6MWD
- patients for whom hospitalization would pose significant clinical, social, or financial burden
Moreover, reducing early hospitalization has ripple effects: fewer emergency evaluations, less reliance on rescue therapies, decreased exposure to inpatient risks, and reduced long-term right ventricular damage. These benefits extend beyond the PAH clinic and influence the broader healthcare system.
The article emphasizes one point particularly well: the goal of therapy in PAH is not merely to treat symptoms, but to alter disease biology. AMBITION demonstrates that initial combination therapy does precisely that.
Conclusion
The AMBITION trial and its detailed hospitalization analysis offer compelling, practice-changing evidence that initial ambrisentan–tadalafil combination therapy significantly reduces the risk, frequency, and early occurrence of PAH-related hospitalizations. By targeting complementary pathophysiologic mechanisms, dual therapy provides structural, hemodynamic, and symptomatic benefits that monotherapy cannot match.
These findings affirm a paradigm shift in PAH management—from stepwise escalation to early, decisive intervention. For patients, this translates to more time at home, less time in hospital beds, and a better chance of maintaining functional independence. For clinicians, it provides confidence that early combination therapy is not only safe but strategically advantageous. And for the healthcare system, reduced hospitalization means improved efficiency, reduced costs, and enhanced long-term outcomes.
In PAH, timing is as critical as therapy choice. AMBITION makes one message unmistakably clear: start strong, start early, and start with combination therapy whenever appropriate.
FAQ
1. Is initial combination therapy suitable for all patients with newly diagnosed PAH?
Most WHO functional class II–III patients benefit from initial combination therapy. However, patients with advanced comorbidities or contraindications to either agent may require individualized adjustments.
2. Why does combination therapy reduce hospitalization more than monotherapy?
Because ambrisentan and tadalafil target distinct mechanisms of pulmonary vascular disease, their combined effects slow disease progression, improve hemodynamics, and strengthen right ventricular resilience, thereby reducing decompensation events that lead to hospitalization.
3. Are adverse effects more common with combination therapy?
Slightly, but not clinically significantly. Most side effects are mild and manageable. The tolerability of the combination regimen in AMBITION was comparable to monotherapy.