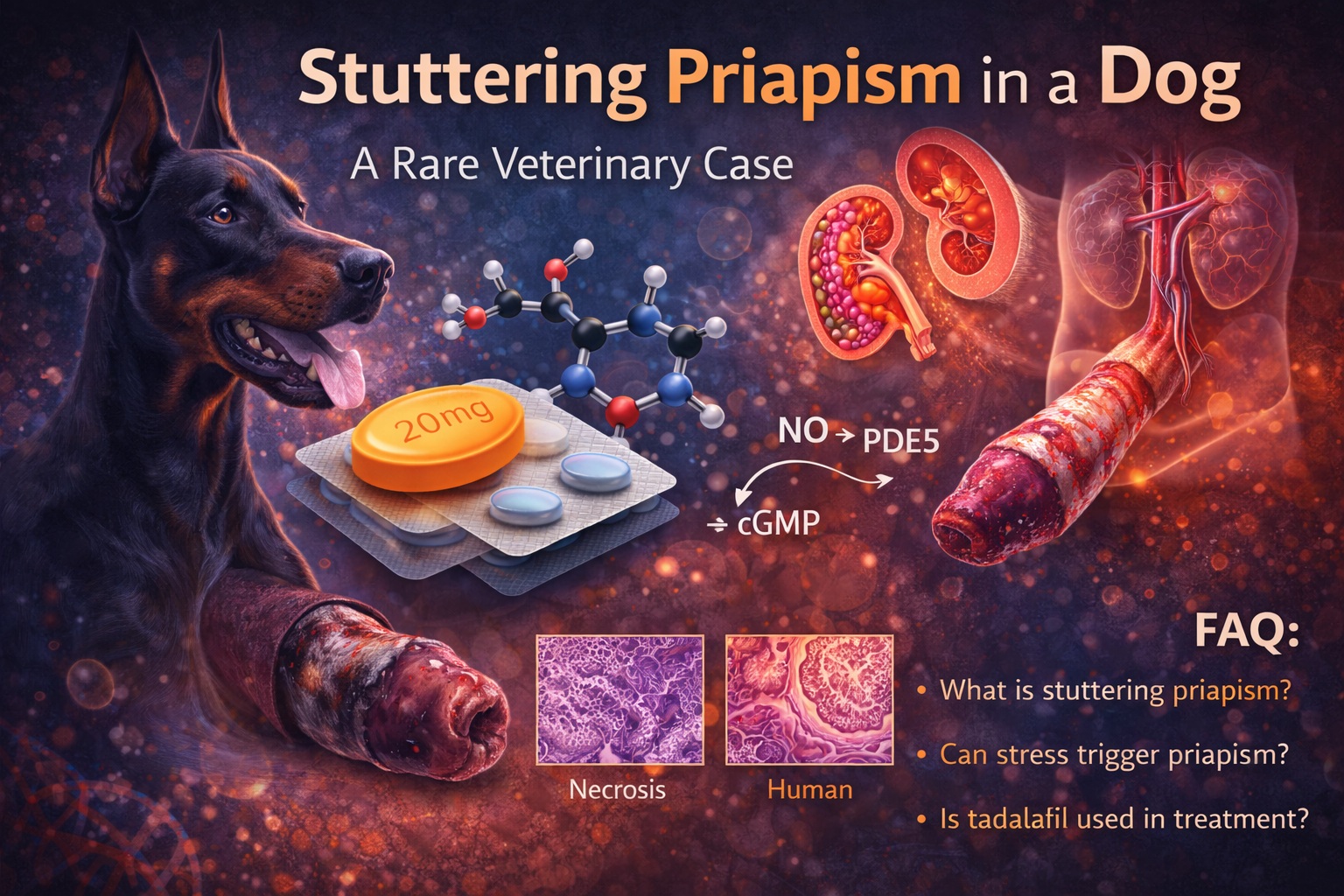
Introduction: When a Rare Case Redefines a Familiar Condition
Priapism is a term that most clinicians associate with human urology, occasionally encountered, rarely welcomed, and always urgent. Defined as a prolonged erection unrelated to sexual stimulation, it represents a failure of the finely tuned mechanisms governing penile detumescence. While well described in human medicine, its occurrence in veterinary practice is uncommon—and its recurrent form, known as stuttering priapism, is even more elusive.
The case described in the source article introduces the first documented instance of stuttering priapism in a dog, expanding the boundaries of both veterinary and comparative medicine . At first glance, this may appear to be a niche observation. In reality, it offers a valuable lens through which we can better understand the pathophysiology, diagnosis, and management of this condition across species.
This article explores that intersection. It moves from a single clinical case to broader implications, connecting veterinary findings with human urological practice. Along the way, it highlights a central truth of medicine: rare cases often illuminate common mechanisms.
Understanding Priapism: A Failure of Physiological Balance
Erection is not a simple hydraulic event; it is a coordinated neurovascular process involving the central nervous system, autonomic regulation, and vascular dynamics. Under normal conditions, parasympathetic activation increases arterial inflow, while venous outflow is temporarily restricted, producing rigidity. Detumescence, in turn, requires sympathetic activation and restoration of venous drainage.
Priapism occurs when this balance is disrupted. Either arterial inflow becomes excessive, or—more commonly—venous outflow is impaired. The result is a persistent erection that fails to resolve, often accompanied by pain and tissue hypoxia.
The distinction between ischemic and non-ischemic priapism is critical. Non-ischemic (high-flow) priapism is typically painless and often self-limiting. Ischemic (low-flow) priapism, by contrast, is a true medical emergency. As emphasized in the source text, ischemic episodes account for the vast majority of cases and are associated with reduced venous return and tissue oxygenation .
This distinction is not academic. It determines both prognosis and treatment strategy. Failure to recognize ischemic priapism in time can lead to irreversible tissue damage within 24–48 hours—a window that is unforgiving and clinically decisive.
The Case That Changed the Conversation
The reported case involves a five-year-old Doberman dog presenting with prolonged penile erection, pain, and urinary difficulty. Notably, this was not an isolated event. The dog had experienced multiple prior episodes, each associated with stress, and each resolving spontaneously—until the final episode.
By the time of presentation, the condition had persisted for seven days. Clinical examination revealed a rigid, painful, darkened penis with no detectable blood flow on Doppler ultrasound—hallmarks of ischemic priapism .
What followed was both dramatic and instructive. Despite supportive measures, the extent of tissue necrosis necessitated complete penile amputation and urethrostomy. Histological analysis confirmed widespread necrosis and hemorrhage, with no evidence of neoplasia.
This outcome underscores a fundamental principle: time matters. The progression from reversible ischemia to irreversible necrosis is not gradual—it is precipitous. The case serves as a stark reminder that delayed intervention carries significant consequences.
Stuttering Priapism: A Pattern of Recurrence
What distinguishes this case from previously reported veterinary cases is the recurrent nature of the episodes. Stuttering priapism, also known as intermittent or recurrent priapism, is characterized by repeated, self-limiting episodes of prolonged erection.
In humans, these episodes often occur during sleep, last less than three hours, and resolve spontaneously. However, over time, they may increase in frequency and duration, culminating in a major ischemic event requiring emergency treatment .
The dog in this case followed a similar trajectory. Early episodes resolved without intervention, creating a false sense of benignity. Yet each episode likely contributed to cumulative vascular dysfunction, ultimately leading to a catastrophic event.
This pattern highlights a subtle but important clinical challenge. Stuttering priapism may initially appear harmless, but it carries the risk of progression. Recognizing this risk is essential for timely intervention and prevention.
Stress, Neurobiology, and the Triggering Mechanism
One of the most intriguing aspects of the case is the consistent association between priapism episodes and stress. Each episode occurred during periods of anxiety, such as owner absence or environmental change.
This observation raises important questions about the role of the autonomic nervous system. Erection and detumescence are regulated by a balance between parasympathetic and sympathetic activity. Stress, by altering this balance, may disrupt normal control mechanisms.
In humans, similar associations have been reported. Anxiety disorders have been identified in a significant proportion of patients with idiopathic priapism, suggesting a possible neuropsychological component .
The implication is that priapism is not solely a vascular disorder. It is also a neurovascular phenomenon, influenced by psychological and environmental factors. This broader perspective may open new avenues for both prevention and treatment.
Diagnostic Strategy: Seeing Beyond the Obvious
Accurate diagnosis of priapism requires more than visual inspection. It demands a systematic approach to differentiate between ischemic and non-ischemic forms, as well as to exclude conditions such as paraphimosis.
Key diagnostic tools include Doppler ultrasound, which assesses blood flow, and clinical evaluation of pain, rigidity, and tissue color. In the reported case, the absence of blood flow on Doppler imaging confirmed the ischemic nature of the condition .
Laboratory tests, while often normal, may help exclude underlying systemic causes. Imaging studies can identify structural abnormalities, though they are frequently unremarkable in idiopathic cases.
The challenge lies not in performing these tests, but in interpreting them within the clinical context. Priapism is a diagnosis that requires both technical skill and clinical judgment.
Management Principles: From Emergency to Prevention
The management of ischemic priapism follows a stepwise approach, beginning with conservative measures and progressing to invasive interventions if necessary. The primary goal is to restore blood flow and prevent tissue damage.
Initial treatment typically involves aspiration of blood from the corpora cavernosa, often combined with intracavernosal injection of sympathomimetic agents such as phenylephrine. These measures are effective in a significant proportion of cases.
In the reported case, these interventions were not performed, a decision that may have contributed to the progression of necrosis . This omission highlights the importance of early, guideline-based management.
When conservative measures fail—or when presentation is delayed—surgical intervention becomes necessary. In veterinary practice, penile amputation is a definitive solution, particularly in castrated animals where reproductive function is no longer a concern.
Prevention Strategies: Where Tadalafil Enters the Discussion
Preventing recurrence in stuttering priapism is both challenging and essential. In human medicine, several pharmacological strategies have been explored, including hormonal therapy and neuromodulatory agents.
Among these, PDE5 inhibitors such as tadalafil occupy a paradoxical position. While they are known to facilitate erection, chronic low-dose administration has been shown to stabilize erectile physiology and reduce the frequency of priapism episodes .
The mechanism is not fully understood but is thought to involve normalization of nitric oxide signaling and improved regulation of smooth muscle tone. In essence, tadalafil may help restore the balance that is disrupted in priapism.
This dual role—both as a facilitator and regulator—reflects the complexity of the underlying physiology. It also serves as a reminder that pharmacological effects are rarely one-dimensional.
Comparative Insight: What Veterinary Medicine Teaches Human Medicine
The significance of this case extends beyond veterinary practice. It provides a unique opportunity to observe priapism in a different biological context, free from some of the confounding factors present in human patients.
Animal models have long contributed to our understanding of disease, but spontaneous clinical cases offer a different kind of insight—one that is grounded in real-world complexity. The parallels between this canine case and human stuttering priapism are striking.
They suggest that the underlying mechanisms are conserved across species, reinforcing the validity of existing pathophysiological models. At the same time, they highlight the need for a multidisciplinary approach that integrates veterinary and human medicine.
Conclusion: A Rare Case with Lasting Implications
Stuttering priapism is a condition that challenges both diagnosis and management. Its recurrent nature, variable presentation, and potential for progression make it a clinical puzzle—one that demands vigilance and expertise.
The case described in the source article adds a new dimension to this puzzle. It demonstrates that the condition is not limited to humans and that its mechanisms may be more universal than previously thought.
For clinicians, the lessons are clear. Early recognition, prompt intervention, and thoughtful prevention are essential. For researchers, the case opens new avenues for exploration, particularly in the realm of neurovascular regulation.
And for all of us, it serves as a reminder that even the rarest cases can teach us something profound.
FAQ: Key Questions About Stuttering Priapism
1. What is stuttering priapism?
It is a recurrent form of ischemic priapism characterized by repeated episodes of prolonged erections.
2. Why is ischemic priapism considered an emergency?
Because prolonged ischemia can lead to irreversible tissue damage within 24–48 hours.
3. Can stress trigger priapism?
Yes, stress may disrupt autonomic regulation and contribute to episodes, as observed in both animals and humans.
4. How is recurrence prevented?
Options include hormonal therapy, neuromodulators, and in some cases PDE5 inhibitors like tadalafil.
5. What is the most important factor in treatment success?
Timing. Early intervention significantly improves outcomes and may prevent irreversible damage.