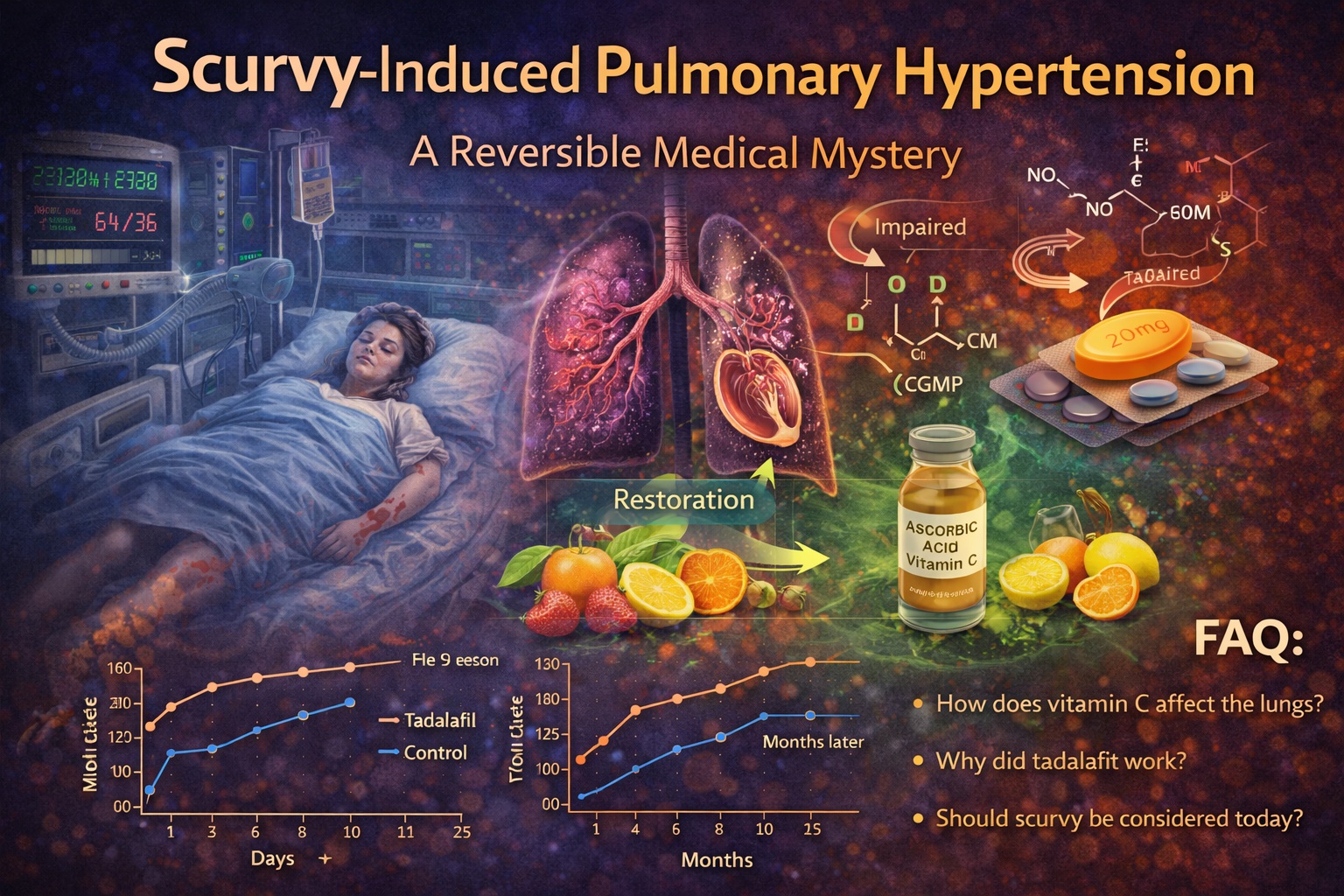
Introduction: A 21st-Century Disease with 18th-Century Roots
Pulmonary hypertension (PH) is a diagnosis that commands urgency. It evokes images of progressive vascular remodeling, right heart failure, and complex, often lifelong therapy. Clinicians are trained to think in terms of idiopathic pulmonary arterial hypertension, chronic thromboembolic disease, or connective tissue disorders. Rarely—almost never—does vitamin deficiency enter the differential.
And yet, it should.
The case presented in the source article describes a young woman in cardiogenic shock, diagnosed with severe precapillary pulmonary hypertension, who experienced a dramatic clinical improvement within hours of receiving tadalafil—and complete resolution after vitamin C supplementation . The underlying cause was not genetic, autoimmune, or thrombotic. It was scurvy.
This is not merely a clinical curiosity. It is a reminder that even in modern medicine, fundamental nutritional deficiencies can masquerade as advanced cardiopulmonary disease. More importantly, they can be rapidly reversible—if recognized.
Clinical Presentation: When Pulmonary Hypertension Appears Overnight
The patient was a 22-year-old woman with a history notable not for chronic disease, but for dietary restriction. Her diet—consisting almost exclusively of beef, eggs, and rice—contained virtually no vitamin C. Over time, this seemingly benign habit set the stage for a profound metabolic disturbance.
Her presentation was acute and severe. Within a week, she developed progressive dyspnea, pleuritic chest pain, and signs of systemic hypoperfusion. On admission, she was hypotensive, tachycardic, and in cardiogenic shock. Laboratory findings included elevated lactate, renal dysfunction, and markedly increased NT-proBNP levels .
Echocardiography revealed a classic picture of right heart strain: severe right ventricular dilation, septal deviation, and underfilling of the left ventricle. Hemodynamic measurements confirmed precapillary pulmonary hypertension, with a mean pulmonary artery pressure of 45 mm Hg and a pulmonary vascular resistance exceeding 13 Wood units.
This was not subtle disease. It was advanced, life-threatening, and—at least initially—indistinguishable from idiopathic pulmonary arterial hypertension.
The Diagnostic Turning Point: A Clue Hidden in Plain Sight
In complex cases, diagnosis often hinges on small details. Here, the turning point came not from imaging or hemodynamics, but from history—specifically, diet.
The patient’s restrictive eating pattern raised suspicion for nutritional deficiency. Additional physical findings, including a perifollicular hemorrhagic rash, supported this hypothesis. Laboratory confirmation followed: her serum vitamin C level was nearly undetectable (<2 μmol/L) .
This finding reframed the entire clinical picture. What appeared to be idiopathic pulmonary hypertension was, in fact, secondary to a reversible metabolic deficiency.
The importance of this shift cannot be overstated. It transformed the management strategy from long-term disease control to targeted correction of an underlying cause. In doing so, it changed the patient’s prognosis from uncertain to excellent.
Pathophysiology: The Nitric Oxide Connection
To understand how scurvy leads to pulmonary hypertension, one must look beyond collagen synthesis—the classical role of vitamin C—and consider its impact on vascular biology.
Vitamin C is essential for endothelial nitric oxide (NO) production. NO is a key regulator of vascular tone, promoting vasodilation through activation of cyclic guanosine monophosphate (cGMP). In its absence, this pathway becomes impaired.
The result is a state of functional vasoconstriction. Pulmonary arterioles, deprived of NO signaling, constrict and increase vascular resistance. Over time, this may be accompanied by structural changes, including increased stiffness and microvascular remodeling .
This mechanism is strikingly similar to that observed in pulmonary arterial hypertension, albeit driven by a different upstream cause. It highlights an important principle: diverse etiologies can converge on common pathophysiological pathways.
Tadalafil: A Pharmacological Clue to the Underlying Mechanism
One of the most remarkable aspects of this case is the patient’s rapid response to tadalafil. Within two hours of receiving a single oral dose, she reported significant improvement in dyspnea and systemic perfusion .
This response was not coincidental—it was diagnostic.
Tadalafil inhibits phosphodiesterase type 5 (PDE5), preventing the breakdown of cGMP and thereby enhancing NO-mediated vasodilation. In a system where NO production is impaired but not absent, this mechanism can partially restore vascular function.
The immediate clinical improvement suggests that the patient’s pulmonary hypertension was driven predominantly by functional vasoconstriction rather than fixed structural changes. In other words, the disease was reversible.
This observation also reinforces the central role of the NO–cGMP pathway in pulmonary vascular physiology. When this pathway is disrupted, even a vitamin deficiency can produce severe hemodynamic consequences.
Vitamin C Therapy: The Definitive Treatment
While tadalafil provided rapid symptomatic relief, it was vitamin C supplementation that addressed the root cause. Following initiation of therapy, the patient’s recovery was swift and complete.
Within 48 hours, her renal function improved, lactate levels normalized, and vasopressor support was reduced. By day four, echocardiography showed normalization of right ventricular size and function .
The echocardiographic images on page 3 illustrate this transformation vividly. Initial images show a dilated right ventricle and septal shift, while follow-up images demonstrate restored cardiac geometry and function.
Three months later, her cardiac function remained normal, confirming sustained recovery. This timeline underscores the reversibility of scurvy-induced pulmonary hypertension when treated appropriately.
Scurvy in Modern Medicine: An Underrecognized Reality
It is tempting to view scurvy as a relic of maritime history, confined to sailors and textbooks. In reality, it persists—often quietly—in modern populations.
Studies have shown that a significant proportion of hospitalized patients have subnormal vitamin C levels, with a smaller but meaningful percentage meeting criteria for deficiency . Risk factors include restrictive diets, malabsorption, chronic illness, and socioeconomic barriers.
The patient in this case exemplifies a growing demographic: individuals with highly selective diets, often for medical or personal reasons, who may inadvertently exclude essential nutrients.
The lesson is clear. Nutritional assessment is not optional—it is integral to clinical evaluation. Even in advanced healthcare settings, basic deficiencies can have profound consequences.
Differential Diagnosis: Expanding the Clinical Perspective
Pulmonary hypertension is traditionally classified into five groups based on etiology. Scurvy-induced PH does not fit neatly into these categories but is best considered within Group 5—conditions with multifactorial or unclear mechanisms.
This classification has practical implications. It encourages clinicians to consider atypical causes when standard evaluations fail to identify a clear etiology.
In this context, vitamin C deficiency should be included in the differential diagnosis of unexplained precapillary pulmonary hypertension, particularly in patients with dietary risk factors.
Other nutritional deficiencies, such as thiamine deficiency, may also influence pulmonary vascular function, although they were not implicated in this case .
Clinical Lessons: What This Case Teaches Us
This case offers several important insights for clinical practice. First, it demonstrates that severe pulmonary hypertension can be rapidly reversible when caused by a functional, rather than structural, disturbance.
Second, it highlights the diagnostic value of therapeutic response. The rapid improvement following tadalafil administration provided a clue to the underlying mechanism, guiding further investigation.
Third, it reinforces the importance of comprehensive history-taking. Dietary habits, often overlooked, can hold the key to diagnosis.
Finally, it challenges assumptions. Not all cases of pulmonary hypertension require lifelong therapy. Some require only the recognition of a correctable cause.
Conclusion: When Simplicity Outpaces Complexity
Modern medicine is often defined by its complexity—advanced imaging, molecular diagnostics, and targeted therapies. Yet, as this case illustrates, the solution to a life-threatening condition may be as simple as vitamin supplementation.
The interplay between scurvy, nitric oxide deficiency, and pulmonary hypertension reveals a fascinating convergence of nutrition and vascular biology. It also underscores the importance of maintaining a broad differential diagnosis, even in seemingly straightforward cases.
Tadalafil, in this scenario, served not only as a therapeutic agent but as a diagnostic tool, illuminating the pathophysiological mechanism at play.
In the end, the lesson is both humbling and empowering: sometimes, the most effective treatment is not the newest drug, but the correct diagnosis.
FAQ: Key Questions About Scurvy and Pulmonary Hypertension
1. Can vitamin C deficiency really cause pulmonary hypertension?
Yes. It can impair nitric oxide production, leading to pulmonary vasoconstriction and increased vascular resistance.
2. Why did tadalafil work so quickly in this case?
It enhanced cGMP signaling, partially restoring vasodilation despite impaired nitric oxide production.
3. Is scurvy still relevant in modern medicine?
Absolutely. It can occur in patients with restrictive diets, malabsorption, or poor nutritional intake.
4. How quickly can recovery occur after treatment?
Clinical improvement can begin within hours to days, with full recovery possible in weeks.
5. Should vitamin deficiencies be routinely checked in pulmonary hypertension?
In unexplained cases—especially with dietary risk factors—yes, they should be considered.