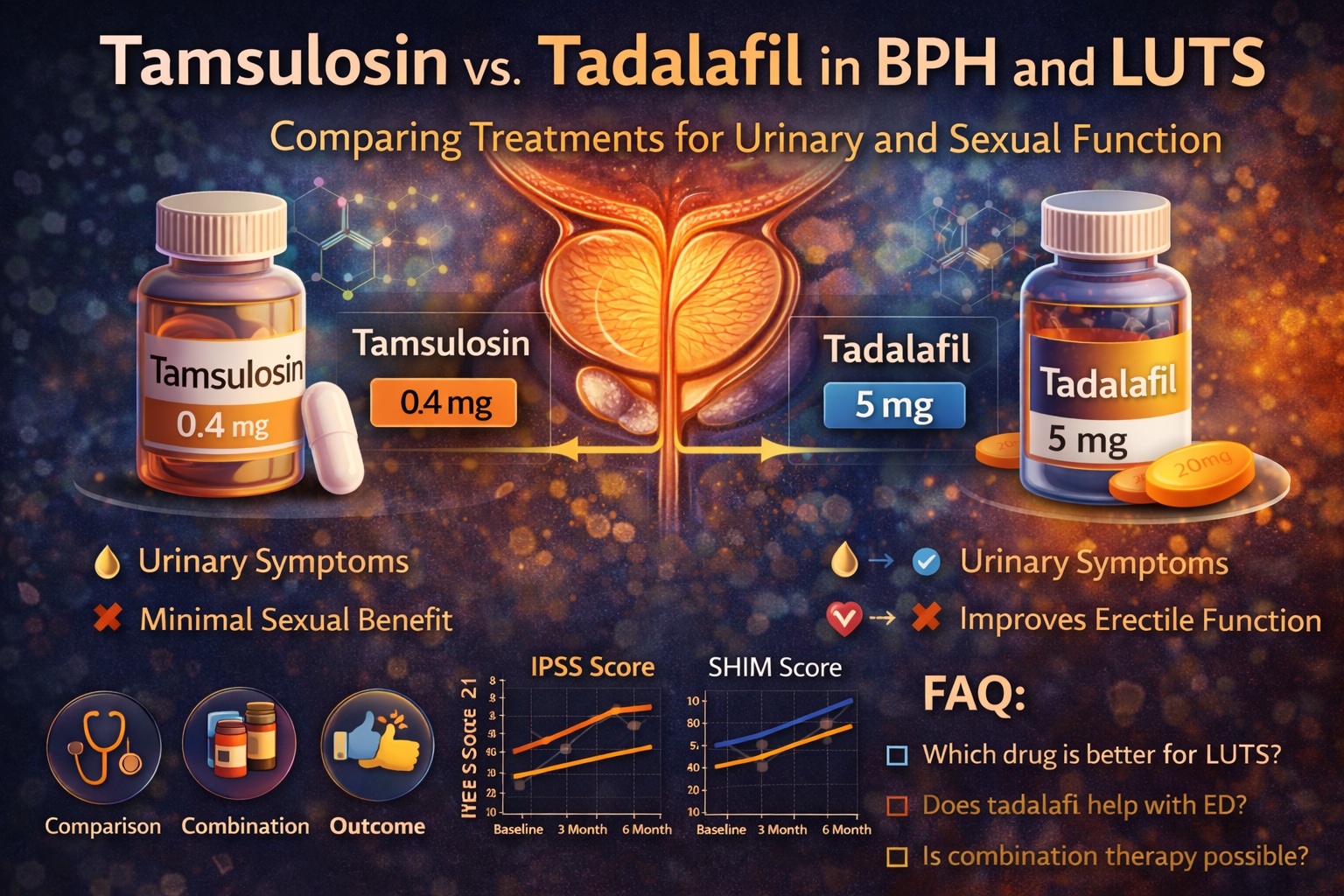
Introduction: When One Disease Becomes Two Problems
Benign prostatic hyperplasia (BPH) is often presented as a simple anatomical issue—an enlarged prostate obstructing urinary flow. In reality, it is a far more complex and multifaceted condition. For the aging male patient, BPH rarely travels alone. It brings with it lower urinary tract symptoms (LUTS), sleep disruption, psychological distress, and—almost inevitably—erectile dysfunction.
The clinical challenge is not merely to improve urinary flow, but to restore quality of life. Historically, treatment strategies have focused on relieving obstruction. Yet modern urology increasingly recognizes that sexual health is not a secondary concern—it is central to patient well-being.
The study analyzed here offers a compelling comparison between two pharmacological approaches: the traditional alpha-blocker tamsulosin and the increasingly versatile PDE5 inhibitor tadalafil. The findings challenge conventional hierarchies and suggest that treatment success depends not only on urodynamics, but on the broader human experience of the patient .
BPH and LUTS: Beyond Mechanical Obstruction
BPH is one of the most common conditions affecting men over the age of 40. It is characterized by nonmalignant enlargement of the prostate, which can compress the urethra and disrupt normal urinary flow.
However, the relationship between prostate size and symptoms is not always linear. As noted in the study, voiding symptoms may or may not correlate directly with anatomical obstruction . This discrepancy highlights the role of additional factors, including smooth muscle tone, inflammation, and neural regulation.
LUTS encompass both obstructive and irritative symptoms. Patients may experience weak stream, hesitancy, incomplete emptying, urgency, and nocturia. These symptoms often coexist and fluctuate over time, creating a dynamic clinical picture.
Importantly, LUTS are not isolated from sexual health. They are independently associated with erectile dysfunction, forming a bidirectional relationship that compounds patient distress. Treating one without addressing the other is, at best, incomplete medicine.
Pharmacological Approaches: Two Mechanisms, One Goal
The management of BPH has evolved significantly over the past decades. Medical therapy is now the first-line approach for most patients, with surgery reserved for refractory cases.
Tamsulosin represents the classical approach. As a selective α1-adrenergic receptor antagonist, it relaxes smooth muscle in the prostate and bladder neck, reducing resistance to urinary flow. Its effects are rapid and well established.
Tadalafil, by contrast, represents a more integrative approach. As a PDE5 inhibitor, it enhances nitric oxide signaling, leading to smooth muscle relaxation not only in the corpus cavernosum, but also in the lower urinary tract. This dual action allows it to address both LUTS and erectile dysfunction simultaneously .
The contrast between these two drugs is not merely pharmacological—it is conceptual. Tamsulosin targets obstruction. Tadalafil targets function.
Study Design: A Balanced Comparison
The study was conducted as a prospective, randomized trial involving 92 patients with symptomatic BPH. After exclusions, 87 patients completed the study, divided into two groups: one receiving tamsulosin 0.4 mg and the other tadalafil 5 mg daily .
Patients were evaluated at baseline, 3 months, and 6 months using a combination of objective and subjective measures:
- Maximum urinary flow rate (Qmax)
- Post-void residual urine (PVR)
- International Prostate Symptom Score (IPSS)
- Sexual Health Inventory for Men (SHIM)
Baseline characteristics were comparable between groups, ensuring a fair comparison. The table on page 3 confirms similar age, prostate size, and symptom severity across both cohorts.
This methodological balance strengthens the validity of the findings and allows for meaningful interpretation.
Urinary Outcomes: Comparable Efficacy with Subtle Differences
Both tamsulosin and tadalafil demonstrated significant improvements in urinary parameters over the six-month period. Qmax increased in both groups, indicating improved urinary flow.
According to the data, tamsulosin produced a slightly greater increase in Qmax—from baseline to 20.88 mL/s at 6 months—compared to 18.92 mL/s in the tadalafil group . Similarly, reductions in post-void residual urine were observed in both groups, with marginally better outcomes in the tamsulosin cohort.
However, these differences were not statistically significant. The results table on page 3 clearly shows that P-values for Qmax and PVR comparisons exceeded 0.05, indicating comparable efficacy.
IPSS scores, reflecting patient-reported symptom severity, also improved in both groups. Again, tamsulosin showed slightly greater improvement, but without statistical significance.
The conclusion is clear: in terms of urinary function, both drugs are effective, and neither holds a decisive advantage.
Sexual Function: Where Tadalafil Changes the Narrative
The most striking difference between the two treatments lies in their impact on sexual function. While tamsulosin produced minimal improvement in SHIM scores, tadalafil demonstrated a dramatic and statistically significant effect.
At 6 months, SHIM scores increased from baseline to 22.1 in the tadalafil group, compared to only 16.3 in the tamsulosin group . This difference was highly significant (P < 0.001), as shown in the comparative table on page 3.
This finding is not surprising, given tadalafil’s mechanism of action. However, its clinical importance cannot be overstated. Erectile dysfunction is not merely a comorbidity—it is a central concern for many patients.
By addressing both LUTS and ED, tadalafil offers a more holistic treatment approach. It does not simply improve urinary flow—it restores a dimension of life that is often overlooked.
Mechanistic Insights: Why the Differences Matter
The differing outcomes between tamsulosin and tadalafil can be understood through their mechanisms of action.
Tamsulosin acts primarily on α1 receptors in the prostate, reducing smooth muscle tone and improving flow. Its effects are localized and mechanical.
Tadalafil, on the other hand, operates through the nitric oxide–cGMP pathway. This pathway is present in multiple tissues, including the bladder, prostate, and penile vasculature. By enhancing cGMP levels, tadalafil promotes smooth muscle relaxation and improves blood flow.
Additionally, tadalafil has been shown to exert anti-inflammatory effects on prostatic tissue, potentially reducing fibrosis and long-term progression of BPH .
This broader mechanism may explain its dual efficacy. It is not simply treating symptoms—it is modulating underlying physiology.
Clinical Implications: Choosing the Right Patient
The findings of this study have direct implications for clinical practice. They suggest that treatment selection should be individualized based on patient priorities and comorbidities.
Two general profiles emerge:
- Patients primarily concerned with urinary symptoms may benefit from tamsulosin
- Patients with concurrent erectile dysfunction may derive greater overall benefit from tadalafil
This distinction is not rigid. Many patients fall somewhere in between, and combination therapy may be appropriate in selected cases.
The key is to move beyond a one-size-fits-all approach. BPH is a heterogeneous condition, and its treatment should reflect that complexity.
Limitations and Contextual Interpretation
While the study provides valuable insights, it is not without limitations. The sample size is relatively small, and the follow-up period is limited to six months.
Additionally, the study does not explore combination therapy, which is increasingly used in clinical practice. Nor does it assess long-term outcomes such as disease progression or need for surgery.
Despite these limitations, the consistency of findings across multiple parameters supports the validity of the conclusions.
It is also worth noting that the study reflects real-world clinical conditions, enhancing its relevance to everyday practice.
Conclusion: Toward Integrated Urological Care
The comparison between tamsulosin and tadalafil is not a contest with a single winner. It is a demonstration of two valid approaches to a complex condition.
Tamsulosin remains a reliable and effective treatment for improving urinary flow. Tadalafil, however, offers something more—a bridge between urinary and sexual health.
In an era of patient-centered medicine, this distinction matters. Treatment success is no longer defined solely by objective measures, but by overall quality of life.
And sometimes, the best therapy is not the one that works slightly better on paper, but the one that addresses the patient as a whole.
FAQ: Key Questions About Tamsulosin and Tadalafil in BPH
1. Which drug is better for urinary symptoms?
Both tamsulosin and tadalafil are effective, with no significant difference in most urinary outcomes.
2. Does tadalafil improve erectile function in BPH patients?
Yes. It significantly improves SHIM scores and sexual performance.
3. Can tadalafil replace tamsulosin?
In patients with both LUTS and ED, tadalafil can be a suitable alternative.
4. Is combination therapy possible?
Yes, and it is increasingly used in clinical practice for selected patients.
5. What is the main advantage of tadalafil?
Its ability to treat both urinary symptoms and erectile dysfunction simultaneously.