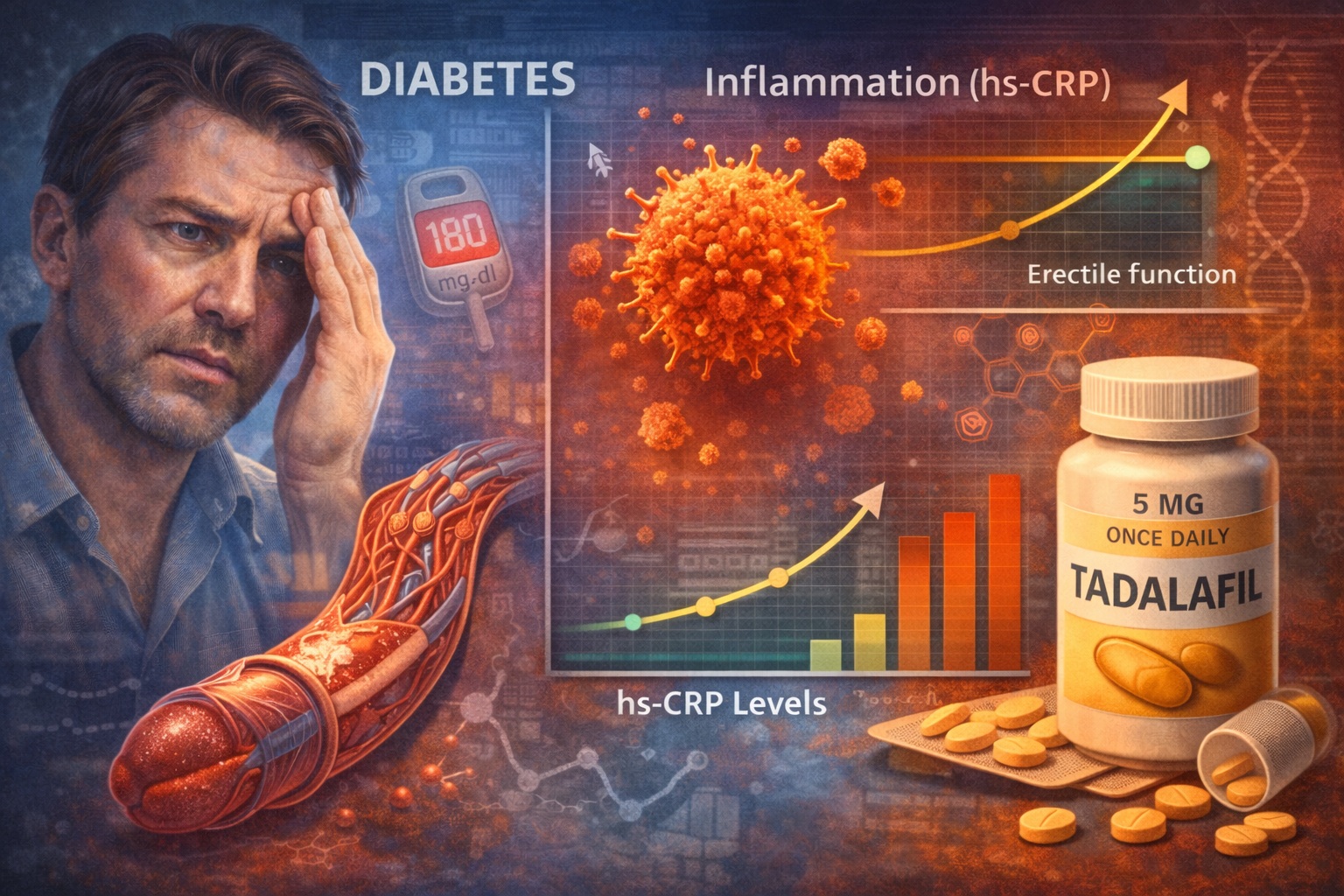
Erectile dysfunction (ED) is often perceived as a localized problem of penile blood flow. In reality, it is frequently a systemic vascular disorder, reflecting deeper disturbances in endothelial function, metabolic health, and inflammatory status. This connection becomes particularly evident in men with diabetes mellitus, where erectile dysfunction occurs earlier, progresses more rapidly, and responds less predictably to therapy.
Among the biological signals linking metabolic disease and vascular dysfunction, high-sensitivity C-reactive protein (hs-CRP) has emerged as a powerful marker of systemic inflammation. Elevated hs-CRP levels are widely recognized as predictors of cardiovascular risk, endothelial dysfunction, and microvascular disease. Unsurprisingly, researchers have begun investigating whether this inflammatory marker may also influence erectile function and treatment response in diabetic patients.
At the same time, phosphodiesterase type-5 (PDE5) inhibitors have become the cornerstone of ED therapy. Among these medications, tadalafil stands out due to its long half-life and the availability of a once-daily dosing regimen. Unlike on-demand medications, daily tadalafil offers continuous modulation of the nitric oxide–cGMP pathway, potentially improving endothelial health over time.
This raises an intriguing question: does systemic inflammation influence how patients respond to tadalafil therapy? And conversely, could successful erectile dysfunction treatment improve vascular health in diabetic individuals?
Recent clinical research examining hs-CRP levels and treatment response to daily tadalafil provides valuable insights into this complex relationship. The findings suggest that erectile dysfunction in diabetes is not simply a mechanical problem—it is an inflammatory vascular condition in which systemic biology and local hemodynamics intersect.
In this article, we explore the relationship between inflammation, erectile dysfunction, and metabolic disease, while examining how daily tadalafil therapy may influence both vascular function and clinical outcomes.
Erectile Dysfunction in Diabetes: A Vascular Disease in Disguise
Diabetes mellitus is one of the strongest risk factors for erectile dysfunction. Studies consistently show that men with diabetes develop ED approximately 10–15 years earlier than the general population. Moreover, diabetic ED tends to be more severe and less responsive to treatment.
The underlying mechanisms are multifactorial. Chronic hyperglycemia damages blood vessels through oxidative stress, endothelial dysfunction, and microvascular injury. Over time, these changes impair the delicate vascular mechanisms responsible for penile erection.
In addition to vascular injury, diabetes also affects neural pathways. Peripheral neuropathy can disrupt the autonomic signals that trigger erectile responses. When both vascular and neural pathways are compromised, erectile dysfunction becomes particularly difficult to treat.
Another critical factor is endothelial dysfunction, which plays a central role in both diabetes and ED. The endothelium is responsible for releasing nitric oxide, the key mediator of penile smooth muscle relaxation. In diabetic patients, nitric oxide production is reduced, and oxidative stress accelerates its degradation.
The result is a physiological environment in which the erectile mechanism becomes inefficient. Even when sexual stimulation occurs, the vascular response is blunted and insufficient to produce a full erection.
From a clinical perspective, erectile dysfunction in diabetic patients often serves as an early warning sign of broader vascular disease. Many cardiologists now view ED as a sentinel symptom of systemic endothelial dysfunction, preceding cardiovascular events by several years.
In other words, when a diabetic patient presents with erectile dysfunction, the issue rarely ends in the bedroom—it often begins in the vascular system.
High-Sensitivity C-Reactive Protein: The Inflammatory Link
High-sensitivity C-reactive protein is a biomarker of systemic inflammation produced by the liver in response to inflammatory cytokines. While CRP has long been used as a general marker of infection or inflammation, high-sensitivity assays allow clinicians to detect even subtle elevations associated with chronic vascular disease.
Elevated hs-CRP levels are strongly associated with atherosclerosis, endothelial dysfunction, and cardiovascular risk. In fact, hs-CRP has become one of the most widely studied biomarkers in preventive cardiology.
In diabetic patients, chronic low-grade inflammation contributes significantly to vascular damage. Hyperglycemia promotes oxidative stress, activates inflammatory pathways, and disrupts endothelial homeostasis. Over time, these processes lead to progressive vascular injury throughout the body.
The penile vasculature is particularly vulnerable to these changes. Penile arteries are smaller than coronary arteries, meaning that even modest vascular impairment can significantly affect blood flow.
This relationship explains why erectile dysfunction frequently appears before other cardiovascular symptoms. In a sense, the penile circulation functions as an early indicator of systemic vascular health.
Researchers have therefore proposed that hs-CRP levels may influence erectile function in several ways:
- Chronic inflammation may impair endothelial nitric oxide production
- Elevated inflammatory cytokines may promote vascular stiffness
- Microvascular circulation may become less responsive to vasodilatory signals
These mechanisms suggest that inflammatory status could potentially influence the effectiveness of PDE5 inhibitor therapy.
Tadalafil and the Nitric Oxide Pathway
Tadalafil belongs to the class of medications known as phosphodiesterase type-5 inhibitors. These drugs work by enhancing nitric oxide–mediated vasodilation within the corpus cavernosum.
When sexual stimulation triggers nitric oxide release, cGMP accumulates within penile smooth muscle cells. This signal causes the smooth muscle to relax, allowing increased arterial blood flow into the erectile tissue.
Phosphodiesterase type-5 normally breaks down cGMP, limiting the duration of the erectile response. By inhibiting PDE5, tadalafil prolongs cGMP activity and amplifies the natural erectile mechanism.
What distinguishes tadalafil from other PDE5 inhibitors is its long half-life, approximately 17 hours. This pharmacokinetic property allows tadalafil to maintain therapeutic activity for more than a day after administration.
For this reason, tadalafil can be prescribed as a once-daily medication at a low dose (5 mg). Daily therapy maintains consistent PDE5 inhibition and may provide continuous endothelial benefits rather than episodic pharmacologic effects.
Some researchers believe that daily tadalafil may improve endothelial health beyond its immediate effect on erectile function. Continuous enhancement of nitric oxide signaling may reduce vascular inflammation and improve microcirculatory function.
This concept has sparked growing interest in the broader vascular benefits of PDE5 inhibitors.
Inflammation and Treatment Response: What the Research Shows
Clinical investigations examining hs-CRP levels in diabetic men with erectile dysfunction have revealed an important pattern: patients with higher baseline inflammatory markers often demonstrate poorer erectile function.
Elevated hs-CRP appears to correlate with greater endothelial impairment and more severe vascular dysfunction. This relationship is not surprising given the central role of inflammation in diabetes-related vascular disease.
When patients receive daily tadalafil therapy, however, interesting changes emerge. In many cases, erectile function improves significantly despite elevated inflammatory markers. This suggests that PDE5 inhibition can partially overcome inflammation-induced vascular dysfunction.
More intriguingly, some studies report reductions in hs-CRP levels following sustained tadalafil therapy. While the exact mechanism remains unclear, improved endothelial function may reduce inflammatory signaling within the vascular system.
These findings raise the possibility that PDE5 inhibitors may exert secondary anti-inflammatory effects through improved vascular physiology.
From a clinical standpoint, the relationship between inflammation and treatment response highlights an important principle: erectile dysfunction therapy in diabetic patients should not focus solely on sexual performance. It should also address systemic metabolic and vascular health.
Clinical Implications for Managing Diabetic Erectile Dysfunction
Treating erectile dysfunction in patients with diabetes requires a comprehensive approach that addresses both metabolic disease and vascular function.
While tadalafil and other PDE5 inhibitors remain first-line therapy, clinicians must also manage the underlying conditions contributing to erectile impairment.
Effective management strategies typically include:
- Optimization of glycemic control
- Treatment of hypertension and dyslipidemia
- Weight management and physical activity
- Smoking cessation and cardiovascular risk reduction
Addressing these factors improves endothelial function and increases the likelihood of successful pharmacologic treatment.
Daily tadalafil therapy offers several advantages in this context. Continuous PDE5 inhibition supports vascular relaxation and may help restore endothelial responsiveness. In diabetic patients, where vascular dysfunction is chronic rather than episodic, daily therapy may provide more consistent benefits than on-demand dosing.
However, clinicians should also recognize that not all patients respond equally. Inflammatory burden, duration of diabetes, and the severity of vascular damage can all influence treatment outcomes.
This variability reinforces the importance of individualized treatment strategies.
Beyond Erectile Function: A Window Into Vascular Health
The relationship between hs-CRP, diabetes, and erectile dysfunction offers a broader lesson about vascular medicine. Erectile function is not an isolated physiological phenomenon; it is a reflection of systemic vascular health.
For many men, erectile dysfunction represents the first clinically noticeable manifestation of endothelial dysfunction. Recognizing this relationship allows clinicians to intervene earlier in the progression of cardiovascular disease.
When a diabetic patient presents with erectile dysfunction, the appropriate response is not merely to prescribe medication. It is also an opportunity to evaluate metabolic control, cardiovascular risk, and inflammatory status.
In this context, tadalafil serves not only as a treatment for ED but also as a tool for restoring vascular signaling pathways impaired by chronic metabolic disease.
The penis, it turns out, is not just an organ of reproduction—it is a remarkably sensitive barometer of vascular health.
FAQ
What is high-sensitivity C-reactive protein and why is it important?
High-sensitivity C-reactive protein (hs-CRP) is a blood marker that reflects low-grade systemic inflammation. Elevated levels are associated with cardiovascular disease, endothelial dysfunction, and metabolic disorders such as diabetes.
Does inflammation affect erectile dysfunction treatment?
Yes. Chronic inflammation can impair endothelial function and reduce nitric oxide availability, making erections more difficult to achieve. Higher inflammatory markers may also influence how patients respond to treatment.
How does daily tadalafil help diabetic patients with ED?
Daily tadalafil 5 mg enhances nitric oxide signaling continuously, improving blood flow to penile tissue. Over time, this therapy may also support endothelial function and potentially reduce inflammatory markers associated with vascular disease.